NASA Lean Test: Objective Autonomic Testing for POTS and Dysautonomia
The NASA Lean Test is a clinically grounded method used to evaluate how the body regulates heart rate and blood pressure during upright posture. Originally developed through aerospace medicine research following the Apollo missions, it provides objective insight into autonomic function and helps identify conditions such as POTS, orthostatic intolerance, and dysautonomia.
What Is the NASA Lean Test?
The NASA Lean Test is a structured form of orthostatic testing used to assess how the cardiovascular and autonomic nervous systems respond to gravity. By measuring heart rate, blood pressure, and symptom response during a controlled upright posture challenge, the test provides clinically useful insight into how well the body is maintaining circulation when a person moves from rest to standing.
Unlike vague symptom descriptions alone, this test adds objective physiologic data to the evaluation. That matters, because many patients with dizziness, fatigue, brain fog, palpitations, exercise intolerance, or post-concussion autonomic symptoms are told everything is “normal” when standard office screening fails to capture what happens during upright stress.
At NeuroSport, the NASA Lean Test is used as part of a broader clinical evaluation to help determine whether autonomic dysfunction may be contributing to a patient’s symptoms.
Origins in NASA and Aerospace Medicine
The roots of this testing approach trace back to aerospace medicine research conducted after the Apollo missions, when investigators studied how spaceflight affected the body’s ability to tolerate upright posture upon return to Earth. Exposure to microgravity reduces the normal physiologic demands of standing, and returning astronauts often demonstrated impaired orthostatic tolerance.
This line of research helped shape practical ways to assess circulatory adaptation to gravity, including passive standing methods that later informed what is now commonly referred to as the NASA Lean Test. One of the early foundational studies comparing passive standing with other orthostatic stress methods was published by Hyatt, Jacobson, and Schneider in 1975.
This historical connection is more than a fun trivia nugget. It reinforces that the test emerged from serious physiologic research focused on how the human body responds to gravitational stress.
Why the NASA Lean Test Matters
For patients with suspected POTS, orthostatic intolerance, dysautonomia, or post-concussion autonomic dysfunction, symptoms often become worse in the upright position. They may feel lightheaded, shaky, weak, nauseated, cognitively foggy, or simply “off” when standing, yet routine testing may miss the pattern entirely.
The NASA Lean Test matters because it helps answer a simple but clinically important question:
Is the body regulating circulation appropriately during upright posture?
This testing can provide objective evidence of abnormal heart rate response, blood pressure instability, or symptom reproduction under controlled conditions. It helps move the discussion from “the patient says they feel bad” to “here is what the body did during upright physiologic challenge.”
That is a much stronger clinical conversation.
How the NASA Lean Test Is Performed
The NASA Lean Test is designed to create a standardized upright posture challenge while minimizing the assistance normally provided by leg muscle activity. This makes it easier to observe how well the autonomic nervous system maintains blood pressure, heart rate regulation, and overall circulatory stability during standing.
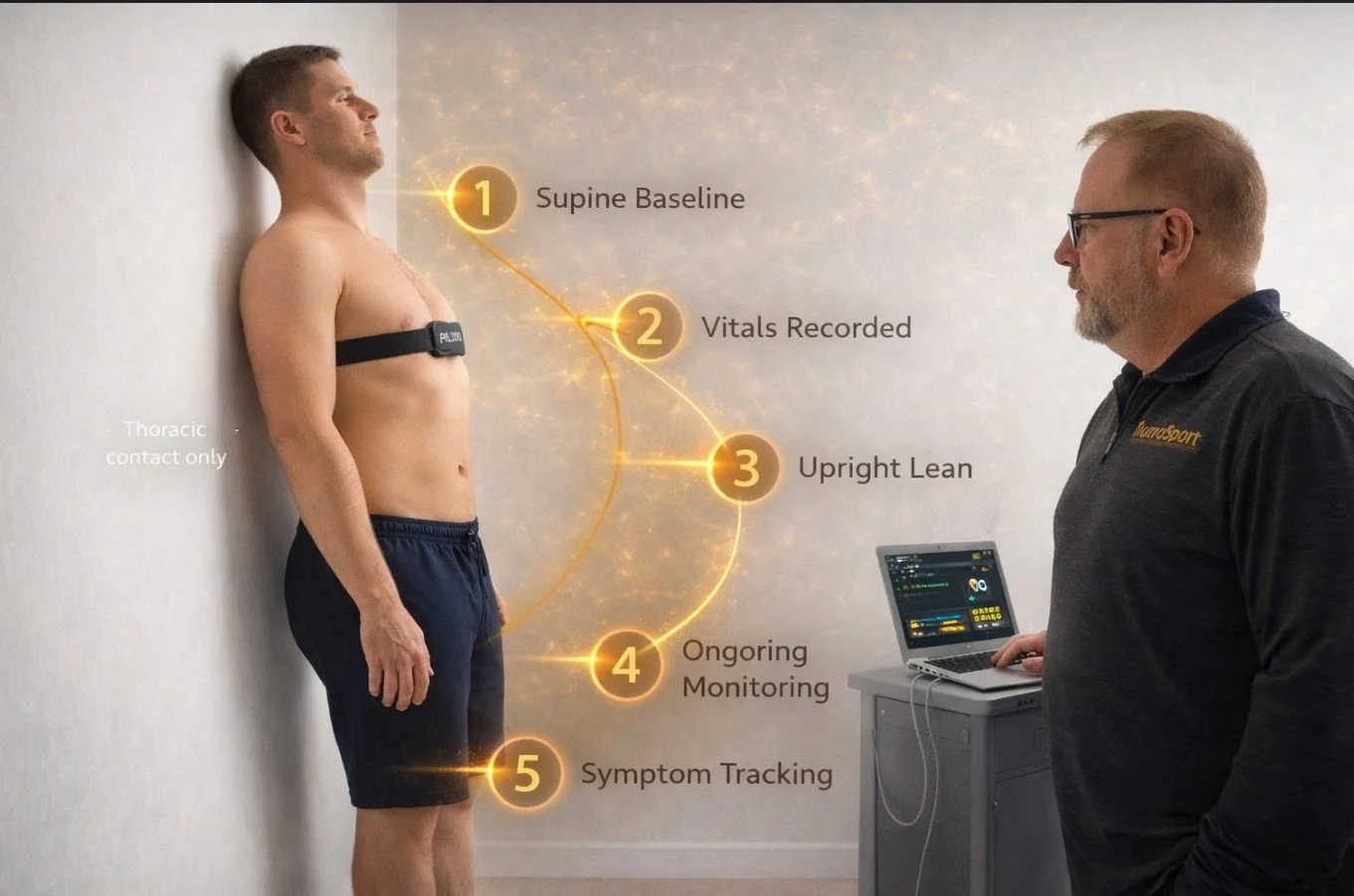
The process generally includes:
A resting supine baseline period
Baseline heart rate and blood pressure measurement
Transition to an upright supported lean position
Repeated heart rate and blood pressure measurements during standing
Ongoing symptom monitoring throughout the test
Because the goal is to evaluate physiologic response to upright posture, the patient’s symptoms during the test are clinically meaningful. A test that reproduces dizziness, lightheadedness, palpitations, visual changes, fatigue, or other orthostatic complaints while objective changes are being recorded can provide valuable diagnostic information.
What We Look For
At NeuroSport, interpretation of the NASA Lean Test goes beyond simply watching the pulse climb and calling it a day. The test is reviewed in the context of both objective physiologic change and symptom behavior.
Key findings may include:
Excessive heart rate increase with upright posture
Inadequate circulatory compensation
Blood pressure instability or abnormal patterning
Reproduction of orthostatic symptoms during the test
Delayed physiologic or symptom recovery after testing
These findings can help support the presence of orthostatic intolerance, autonomic dysfunction, or a POTS-like presentation when interpreted within the full clinical picture.
One graph never gets to wear the sheriff’s badge by itself. It has to work with the rest of the case.
Example physiologic response during testing:
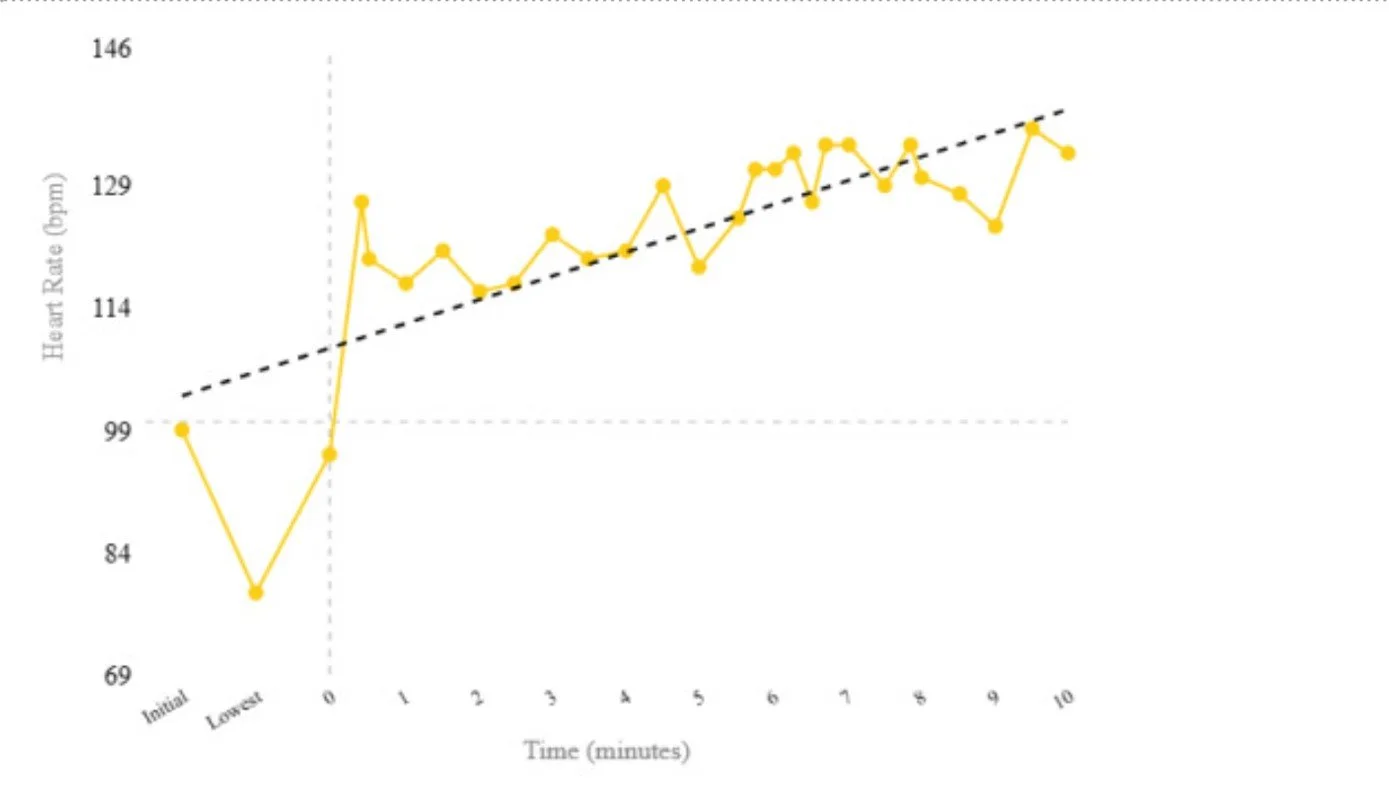
Patterns like this help identify abnormal autonomic responses when interpreted in the full clinical context.
Conditions This Test May Help Evaluate
The NASA Lean Test may be clinically useful in patients with symptoms suggestive of autonomic dysfunction, particularly when symptoms are triggered or worsened by standing.
This may include evaluation of:
Postural Orthostatic Tachycardia Syndrome (POTS)
Orthostatic intolerance
Dysautonomia
Post-concussion autonomic dysfunction
Unexplained dizziness or lightheadedness
Exercise intolerance
Fatigue with upright activity
Palpitations associated with standing
The test is not used in isolation, and it is not intended to replace broader medical evaluation when other causes of symptoms are being considered. It is one piece of a structured diagnostic process.
Clinical Integration at NeuroSport
At NeuroSport, the NASA Lean Test is not treated as a standalone novelty or a one-off data point. It is integrated into a broader clinical framework that may also include neurologic examination, cervical spine assessment, concussion evaluation, oculomotor assessment, symptom profiling, and functional testing.
That matters because complex patients rarely show up with tidy little boxes around their symptoms.
A patient may have:
autonomic dysfunction contributing to dizziness and fatigue
cervical dysfunction contributing to headache or disequilibrium
post-concussion changes affecting exercise tolerance and cognitive load
overlapping musculoskeletal and neurologic factors
The value of the NASA Lean Test is not merely that it measures response to standing. Its value is that it helps clarify whether autonomic dysfunction is part of the symptom picture and how that information should shape the overall care plan.
Why NeuroSport Uses Objective Autonomic Testing
Many patients with suspected dysautonomia or POTS have spent months, and sometimes years, trying to explain symptoms that are variable, poorly understood, and easy for others to dismiss. Objective autonomic testing helps provide a more accurate clinical picture.
At NeuroSport, the NASA Lean Test is used because it helps:
document physiologic response to upright posture
identify autonomic contributors to symptom burden
guide individualized management strategies
monitor change over time
support more precise clinical decision-making
This reflects a core principle of NeuroSport’s approach: identify the actual drivers of symptoms rather than treating everything like generic fatigue, anxiety, or deconditioning.
Not improving with standard testing or care?
Need a more detailed evaluation for suspected POTS, orthostatic intolerance, or autonomic dysfunction?
NeuroSport uses objective physiologic testing, including the NASA Lean Test, as part of a comprehensive clinical evaluation designed to identify the underlying drivers of complex symptoms.
Book an appointment
Call 360-325-2121

