Why You Feel Worse After Eating with Dysautonomia
If you feel worse after eating, you’re not alone — and it’s not in your head
Understanding blood flow, glucose stability, and why your symptoms are not random
Many patients with dysautonomia notice a frustrating pattern:
they feel worse after eating.
You may experience:
lightheadedness
fatigue
brain fog
shakiness
a “crash” 1–2 hours after a meal
This is not random. It is physiology.
In dysautonomia, eating creates a shift in blood flow to the digestive system, reduces blood delivery to the brain, and can trigger rapid changes in blood sugar. Together, these effects place additional stress on an already unstable autonomic nervous system.
The result is a predictable cycle of symptoms that many patients mistakenly believe is unrelated to their condition.
At NeuroSport, we approach nutrition differently.
This page explains why these symptoms occur and how targeted nutrition strategies can help stabilize brain function, improve blood flow, and reduce daily symptom burden.
Why This Happens: The Brain–Blood Flow–Fuel Connection
To understand why symptoms worsen after eating, you need one key concept:
Your brain depends on a constant, stable supply of blood and fuel. In dysautonomia, that system is not stable.
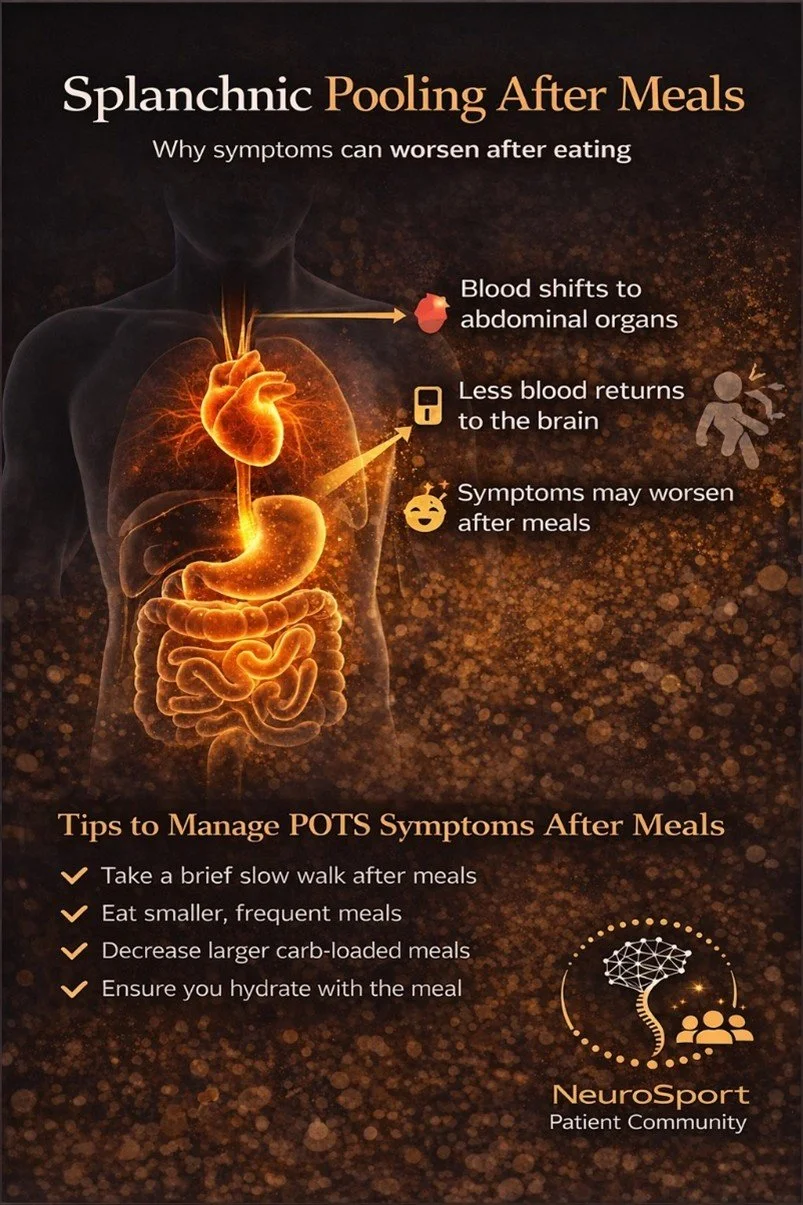
1. Blood Flow Shifts After Eating
When you eat, blood is redirected to the digestive system. That’s normal.
In dysautonomia:
blood vessels do not constrict effectively
more blood pools in the abdomen
less blood returns to the heart and brain
Result:
reduced cerebral perfusion
increased heart rate
lightheadedness and fatigue
2. The Brain Feels It First
The brain is highly sensitive to even small drops in blood flow.
This can cause:
brain fog
poor concentration
visual changes
a sense of pressure or disorientation
Many patients feel mentally worse before they feel physically worse.
3. Glucose Instability Compounds the Problem
Meals, especially higher carbohydrate meals, can create rapid swings in blood sugar:
quick rise in glucose
insulin response
relative drop shortly after
In dysautonomia, this response is exaggerated.
Result:
fatigue
shakiness
anxiety-like symptoms
the “crash” 1–2 hours after eating
4. The Combined Effect
After a meal:
blood shifts away from the brain
glucose levels fluctuate
the autonomic system struggles to compensate
This creates a predictable pattern:
“I feel worse after meals”
“I need to snack constantly”
“I crash in the afternoon”
Key Takeaway
This is not random.
This is not just a heart rate issue.
This is a problem of blood flow regulation and fuel delivery to the brain.
Post-Meal Hemodynamic Response in Dysautonomia
Blood is redirected to the digestive system after eating. In dysautonomia, impaired vascular regulation leads to excessive abdominal pooling, reduced return to the heart and brain, and a compensatory increase in heart rate, contributing to fatigue, brain fog, and lightheadedness.
Why Typical Diet Advice Fails in Dysautonomia
Most nutrition advice assumes a stable system. Dysautonomia is not a stable system. That’s the problem.
1. “Eat Healthy” Is Too Vague
General advice like:
eat balanced meals
avoid processed foods
reduce sugar
is not wrong… it’s just incomplete.
It does not address:
blood pooling after meals
unstable cerebral perfusion
rapid glucose shifts
Patients can “eat healthy” and still feel terrible.
2. Large Meals Make Symptoms Worse
Standard eating patterns often include 2–3 larger meals per day.
In dysautonomia, that backfires:
larger meals → greater blood shift to the gut
increased autonomic demand
reduced blood flow to the brain
Result:
more lightheadedness
more fatigue
post-meal crashes
3. High-Carbohydrate Meals Trigger Instability
Typical diets are often carbohydrate-heavy, especially at breakfast and lunch.
Examples:
cereal
toast
smoothies
energy bars
These can lead to:
rapid glucose spikes
insulin-driven drops
worsening symptoms shortly after
Patients often describe this as:
“I feel worse after I eat”
“I crash mid-day”
4. Low-Carb or Keto Isn’t Always the Answer
Some patients try to “fix” symptoms by cutting carbs aggressively. That can create new problems:
reduced plasma volume
increased fatigue
poor exercise tolerance
The goal is not zero carbs. The goal is controlled, stable fuel delivery.
5. Liquid Calories Are a Common Mistake
Smoothies, juices, and sweetened drinks are often seen as “healthy.” In dysautonomia, they can be problematic:
absorbed rapidly
spike glucose quickly
drop just as fast
They deliver fuel too fast… and then take it away.
Bottom Line: Most diet advice focuses on what you eat.
In dysautonomia, what matters more is:
how much you eat
when you eat
how your body responds
Without that framework, even “good” nutrition can drive symptoms.
Clinical Pearl:
Post-meal symptoms in dysautonomia are often circulatory, not digestive. The underlying issue is impaired autonomic regulation of blood flow, not food intolerance.
The NeuroSport Nutrition Strategy
The goal is simple: Stabilize blood flow and fuel delivery to the brain.
This is not about dieting. This is about controlling physiology.
1. Eat Small, Frequent Meals (Non-Negotiable)
4–6 smaller meals per day
Avoid large meals, especially mid-day
Why this matters:
smaller meals reduce blood shift to the gut
lower autonomic stress
more stable symptoms throughout the day
2. Build Every Meal Around Protein First
Every meal should start with protein.
Target:
~20–30 grams per meal
Then add:
healthy fats
controlled carbohydrates
This slows digestion and stabilizes glucose delivery.
Simple structure:
Protein: eggs, chicken, fish, Greek yogurt
Fats: avocado, olive oil, nuts
Carbs: fruit, vegetables, whole grains (in moderation)
3. Control Carbohydrates (Don’t Eliminate Them)
The goal is stability, not restriction.
avoid large carb loads
never eat carbs alone
pair carbs with protein and fat
Better choices:
berries
sweet potatoes
oats (if tolerated)
quinoa
This helps prevent rapid spikes and crashes.
4. Increase Sodium and Fluids
For many patients, this is essential.
Typical targets (adjust as needed):
fluids: 2–3 liters per day
sodium: 3–8 grams per day
Why:
supports plasma volume
improves blood flow to the brain
reduces orthostatic symptoms
Sources:
electrolyte drinks (low sugar)
salted foods
broths
5. Time Meals Around Activity
This is often overlooked.
eat before activity, not after a crash
avoid large meals before standing-heavy tasks
Better approach: small protein + carb snack before activity
Example:
Greek yogurt with berries before walking or errands
6. Start the Day Correctly
Morning is often the most unstable period.
Avoid:
skipping breakfast
coffee on an empty stomach
Instead:
hydrate first (water + electrolytes)
eat within 30–60 minutes
Example:
eggs, avocado, small fruit
7. Manage “Crash” Patterns
If you feel worse 1–2 hours after eating:
This is often:
relative hypoglycemia
autonomic over-response
Adjust by:
reducing meal size
increasing meal frequency
always pairing carbs with protein/fat
8. Use Caffeine Carefully
Caffeine can help or worsen symptoms.
may improve alertness in some
may trigger tachycardia or anxiety in others
Guidelines:
trial individually
never on an empty stomach
always pair with food
9. Limit Alcohol
Alcohol commonly worsens symptoms:
vasodilation
dehydration
disrupted sleep
Most patients do better reducing or eliminating it.
Bottom Line
If you simplify all of this:
small meals
protein first
controlled carbs
increased salt and fluids
no glucose rollercoasters
Do this consistently, and you reduce a major driver of symptoms.
Foods That Usually Work Better
Patients with dysautonomia often do better with meals that digest steadily, support blood volume, and reduce large swings in glucose.
Examples include:
eggs with avocado and fruit
Greek yogurt with berries and nuts
chicken with rice or sweet potato
salmon with vegetables and olive oil
cottage cheese, apple slices, and nut butter
broth-based meals with added sodium when appropriate
The goal is not a “perfect diet.” The goal is a more stable physiologic response.
Foods and Patterns That Commonly Trigger Symptoms
Many patients notice worse symptoms after foods or meal patterns that create rapid digestion, abrupt glucose shifts, or excessive post-meal blood flow demand.
Common trouble areas include:
very large meals
high-sugar breakfasts
eating carbohydrates by themselves
smoothies or juice without protein
heavily processed snack foods
alcohol
caffeine on an empty stomach
These triggers do not affect every patient the same way, but they are common starting points when symptoms worsen after eating.
A Simple Starting Plan
If you are not sure where to begin, start here for 7 to 10 days:
eat 4 to 6 smaller meals or snacks per day
hydrate early in the day
include protein with every meal
do not eat large amounts of carbohydrates alone
increase sodium and fluids if clinically appropriate
track meals and symptoms for patterns
This simple reset often reveals whether meal size, food composition, or timing is driving symptom flares.
One-Day Sample Structure
This is not a prescription. It is a practical example of how to reduce post-meal crashes.
Morning
Water plus electrolytes, followed by eggs, avocado, and a small piece of fruit
Mid-morning
Greek yogurt with berries or a protein-based snack
Lunch
Chicken, vegetables, and a moderate portion of rice or sweet potato
Mid-afternoon
Cheese, nuts, or a protein snack with a small carbohydrate source
Dinner
Fish or lean protein, vegetables, healthy fat, and a controlled carbohydrate portion
Evening, if needed
A light snack with protein if symptoms tend to worsen later in the day
Keep a Symptom and Food Log
Many patients say, “I feel bad after eating,” but the pattern becomes much clearer when it is tracked.
For 1 to 2 weeks, note:
time of meal
what you ate
how large the meal was
symptoms 30 to 120 minutes later
heart rate changes if you monitor them
whether you were upright, active, or stressed
This helps identify whether the main issue is meal size, carbohydrate load, timing, hydration, or a combination of factors.
Important Clinical Note
Nutrition can help reduce symptom burden, but it is not the entire treatment plan. A focus should be to maintain adequate nutritional stores, including carbohydrates. Low to very low carbohydrate diet may deprive the brain of much needed glucose. Inadequate hydration and electrolyte imbalance are common flare triggers. → Learn how flares develop and how to respond early
If you have dysautonomia or POTS, nutrition works best when combined with a broader strategy that may include:
fluid and electrolyte support
autonomic rehabilitation
graded exercise when appropriate
compression strategies
sleep optimization
targeted medical evaluation when indicated
At NeuroSport, we look at nutrition as one part of stabilizing the full brain-body system.
When to Get Individualized Help
You should not try to figure this out alone if you have:
frequent post-meal crashes
significant dizziness or near-fainting
major fatigue after eating
difficulty maintaining activity tolerance
unexplained shakiness or glucose-like crashes
symptoms that continue despite “eating healthy”
These patterns often require a more specific physiologic approach.
Final Takeaway
If you feel worse after eating, your symptoms are not random and they are not “just anxiety.”
In dysautonomia, meals can expose an unstable system by shifting blood flow, stressing circulation, and disrupting steady fuel delivery to the brain.
The solution is not extreme dieting.
The solution is smarter structure:
smaller meals
protein first
controlled carbohydrates
better hydration and sodium support
fewer glucose swings
less physiologic stress after eating
That is where improvement starts.
Take the Next Step
If post-meal fatigue, dizziness, brain fog, or sudden “crashes” are part of your daily pattern, it is time to look deeper.
At NeuroSport Spine and Concussion Center, we specialize in the evaluation and management of dysautonomia, POTS, and complex post-concussion conditions. Our approach focuses on identifying the underlying physiologic drivers, not just managing symptoms.
A structured plan can make a measurable difference.
Call 360-326-2121 to schedule an evaluation and begin building a strategy tailored to your system.

