
POTS & Dysautonomia Care at NeuroSport
Structured evaluation and targeted care for patients with autonomic dysfunction, persistent symptoms, and complex POTS presentations.
If your symptoms have been difficult to explain, difficult to measure, or difficult to improve, the problem may not be simple.
At NeuroSport, care begins with identifying the systems involved, including autonomic regulation, cardiovascular response, neurologic function, cervical spine contribution, and recovery tolerance.
Many patients we see have already been diagnosed with POTS, suspected of having POTS, or told their symptoms are unclear. Our role is to help define the pattern, identify contributing factors, and guide care based on objective clinical findings.
Does This Sound Like You?
Many patients who come to NeuroSport have already been evaluated, tested, or treated, but their symptoms still do not fully make sense or have not improved.
You feel worse when standing, in heat, or after activity
Your heart rate increases quickly with minimal exertion
You experience dizziness, lightheadedness, or near-fainting episodes
Fatigue does not match your level of activity
Brain fog or difficulty concentrating affects daily function
Symptoms fluctuate and do not follow a consistent pattern
You have been told your testing is “normal,” but you do not feel normal
You suspect POTS or dysautonomia, or have already been diagnosed
These patterns often reflect underlying dysfunction within the autonomic nervous system, but in many cases, multiple systems are contributing at the same time.
POTS is rarely a single-system problem.
What Are POTS and Dysautonomia?
Postural Orthostatic Tachycardia Syndrome (POTS) is a form of dysautonomia, a condition involving dysfunction of the autonomic nervous system. The autonomic nervous system regulates many automatic body functions that occur without conscious effort, including heart rate, blood pressure, circulation, breathing, digestion, temperature regulation, and aspects of recovery and exercise tolerance. The autonomic systems functionality is critical to good health.
When a healthy person changes position from lying down to standing, the body automatically adjusts blood vessel tone, heart rate, and circulation to maintain stable blood pressure and blood flow to the brain and vital organs. In patients with POTS or/and dysautonomia, these regulatory systems may not respond appropriately. Blood may pool excessively in the legs, lower arms or abdomen because blood vessel constriction may become impaired resulting in blood vessel dilation instead of constriction which allows the blood to pool. The autonomic driven “Central Control” communication between the brain, heart, and vascular system frequently becomes dysregulated.
As a result, the blood flow back to the heart decreases, so the body must compensate by increasing heart rate in an attempt to maintain blood flow to the brain. This physiologic stress response can contribute to a wide range of symptoms that may fluctuate significantly throughout the day.
Common symptoms may include:
Dizziness or lightheadedness when standing
Rapid heart rate or palpitations
Fatigue or reduced endurance
Brain fog or difficulty concentrating
Exercise intolerance
Head pressure or headaches
Temperature regulation difficulties
Near-fainting or fainting episodes
Visual disturbances
Gastrointestinal symptoms
Tremulousness or internal shaking sensations
POTS is not a single uniform condition.
In many patients, symptoms reflect multiple interacting physiologic contributors involving the autonomic nervous system, cardiovascular regulation, blood volume control, neurologic function, cervical spine contributions, and recovery tolerance.
At NeuroSport, evaluation focuses not only on identifying the presence of POTS or dysautonomia, but also on understanding the underlying systems contributing to the patient’s presentation. Many patients arrive after prior evaluations have been inconclusive, symptoms have fluctuated unpredictably, or standard approaches have not fully explained the severity or persistence of their condition.
Our goal is to identify the physiologic drivers contributing to symptoms and use that information to guide structured, individualized care.
Why Symptoms Often Fluctuate
Symptoms associated with POTS and dysautonomia often vary from day to day, and sometimes even hour to hour. Patients may feel relatively stable one day and significantly worse the next, even when they feel they have not changed their routine in an obvious way.
Symptoms may worsen with heat exposure, dehydration, illness, poor sleep, emotional stress, hormonal changes, prolonged standing, rapid position changes, large meals, travel, overexertion and many other reasons. Many patients also experience delayed symptom flares after doing too much, where the nervous system tolerates an activity in the moment but struggles to recover afterward.
This variability does not mean symptoms are psychological! It can be frustrating when the symptom complex is inconsistent, or seems imagined. In many, if not most cases, fluctuating symptoms reflect instability within the autonomic nervous system and the body’s ability to regulate circulation, cardiovascular response, temperature control, and physiologic recovery under changing demands.
For a person with dysautonomia, everyday stressors can place a larger-than-normal demand on the system. Standing in a warm environment, walking through a grocery store, sitting upright for a long appointment, or completing normal school or work tasks may require more cardiovascular and neurologic effort than expected. When the system is already under strain, even small additional demands can trigger a symptom flare.
This is why many patients describe dysautonomia as unpredictable. The goal is not only to reduce symptoms, but to identify the patterns, triggers, and physiologic limitations that explain why symptoms worsen. This is also why care must be individualized. At NeuroSport, this helps guide a more structured plan for pacing, hydration, compression, exercise progression, and autonomic rehabilitation.
Common Symptoms of POTS & Dysautonomia
POTS and dysautonomia can affect multiple body systems simultaneously. Symptoms may fluctuate in intensity and are often worsened by upright posture, heat exposure, dehydration, illness, stress, poor sleep, or physical and cognitive overexertion.
Many patients experience symptoms across several physiologic domains rather than a single isolated complaint. Some individuals primarily struggle with dizziness and rapid heart rate, while others may be more affected by fatigue, exercise intolerance, cognitive dysfunction, temperature regulation problems, gastrointestinal symptoms, or delayed recovery after activity.
Common symptoms may include:
Cardiovascular & Circulatory Symptoms
Rapid heart rate upon standing
Heart palpitations
Lightheadedness or dizziness
Near-fainting or fainting episodes
Blood pooling in the legs, hands, or abdomen
Chest discomfort or chest pressure
Shortness of breath
Exercise intolerance
Reduced upright tolerance
Feeling worse after prolonged standing
Cognitive & Neurologic Symptoms
Brain fog
Difficulty concentrating
Slowed processing speed
Memory difficulties
Mental fatigue
Head pressure
Headaches or migraines
Dizziness or disequilibrium
Visual sensitivity or blurred vision
Sensitivity to busy environments or motion
Fatigue & Recovery Symptoms
Persistent fatigue
Reduced stamina
Delayed recovery after activity
Feeling “crashed” after exertion
Non-restorative sleep
Difficulty tolerating normal daily activities
Energy fluctuations throughout the day
Increased symptoms following physical or cognitive overexertion
Temperature & Autonomic Regulation Symptoms
Heat intolerance
Excess sweating or reduced sweating
Cold hands or feet
Temperature sensitivity
Adrenaline surges
Tremulousness or internal shaking sensations
Feeling physically “wired” or overstimulated
Difficulty tolerating hot showers, warm rooms, or summer temperatures
Gastrointestinal & Systemic Symptoms
Nausea
Bloating
Early fullness when eating
Abdominal discomfort
Constipation or gastrointestinal irregularity
Appetite changes
Motion sensitivity
Generalized weakness
Feeling unwell after meals
Not every patient experiences all symptoms, and symptom patterns can vary significantly between individuals. At NeuroSport, evaluation focuses on identifying the physiologic patterns contributing to the patient’s presentation rather than relying solely on a single symptom or isolated measurement.
Why Symptoms Persist
Many patients with POTS and dysautonomia are told their condition is unclear, anxiety-related, or something they must simply learn to manage. In many cases, persistent symptoms reflect underlying dysfunction that has not been fully identified or properly addressed.
Most patients are not dealing with a single problem, they are dealing with interacting systems.
Common Drivers of Persistent Symptoms
Impaired autonomic nervous system regulation
Disruption of communication between the brain and heart (neurocardiac axis)
Abnormal vascular control and blood flow distribution
Cervical spine and sensorimotor contributions
Deconditioning and reduced physiologic tolerance
Volume regulation challenges
What This Means Clinically
When these systems are not functioning properly, the body struggles to maintain stable blood flow, cardiovascular control, and neurologic balance, particularly in the upright position.
This can lead to:
Ongoing dizziness and lightheadedness
Exaggerated heart rate response
Fatigue that does not recover normally
Cognitive symptoms such as brain fog
Symptoms that fluctuate or worsen with activity, heat, or stress
At NeuroSport, evaluation is designed to identify these underlying contributors and guide targeted, system-based care. Persistent symptoms are often treatable when the true drivers are properly identified.
Why POTS Is Often Missed or Misunderstood
POTS and dysautonomia can be difficult to recognize because symptoms often fluctuate, involve multiple body systems, and may not appear abnormal on standard medical testing. Many patients look outwardly healthy while simultaneously struggling with significant physiologic limitations affecting school, work, exercise tolerance, travel, daily activities, or recovery capacity.
Patients commonly report seeing many providers before the larger autonomic pattern is identified. Symptoms may initially appear unrelated or inconsistent because they can involve cardiovascular, neurologic, cognitive, gastrointestinal, vestibular, temperature-regulation, and fatigue-related systems simultaneously.
In most cases, standard imaging studies such as MRI or CT scans may appear normal. Routine laboratory testing may also fail to fully explain symptom severity. This does not mean symptoms are psychological or insignificant. The wrong clinical tools were used to identify the problem. Dysautonomia often involves dysfunction in physiologic regulation rather than structural damage that is easily visualized on traditional imaging.
Symptoms also commonly overlap with stress physiology and anxiety-related responses. When the brain needs to divert precious resources to manage to stress, there are less resources to deal with all the other brain medicated functions. For example, elevated heart rate, sweating, shakiness, chest discomfort, adrenaline surges, and shortness of breath may resemble panic or anxiety presentations. While emotional stress can worsen autonomic symptoms, physiologic dysregulation within the autonomic nervous system may also independently generate many of these same responses.
This overlap can make diagnosis more challenging, particularly when symptoms fluctuate or worsen intermittently. Some patients may feel relatively functional on certain days and significantly limited on others depending upon hydration status, sleep quality, heat exposure, illness, exertion level, hormonal changes, environmental stressors, or upright demands.
Another challenge is that many patients adapt gradually to chronic symptoms over time. Individuals may reduce activity levels, avoid triggering situations, sit more frequently, stop exercising, or unconsciously pace their activities in ways that partially mask the severity of autonomic dysfunction. This is not OK as a new normal. As a result, the full physiologic burden may not always be immediately obvious during a brief office visit.
At NeuroSport, evaluation focuses on identifying the larger physiologic pattern contributing to symptoms rather than viewing complaints as isolated or unrelated problems. This systems-based approach helps guide more individualized evaluation, rehabilitation, activity pacing, autonomic support strategies, and recovery planning.
Not All POTS Patients Are the Same
One of the most important concepts in autonomic medicine is that POTS is not a single uniform disorder. While patients may share certain hallmark symptoms such as rapid heart rate, dizziness, fatigue, exercise intolerance, or brain fog, the underlying physiologic contributors can vary considerably from person to person.
For example, some individuals primarily struggle with fainting and brain fog, while others experience disordered sleep and elevated heart rates. Others demonstrate adrenaline-related symptoms. In some patients, POTS develops following concussion, viral illness, surgery, autoimmune disease, connective tissue disorders, or prolonged physiologic stress. Many, if not most, patients demonstrate overlapping features from multiple subtypes rather than fitting neatly into a single category.
At NeuroSport, evaluation focuses not only on identifying the presence of POTS or dysautonomia, but also on understanding the patterns contributing to the patient’s presentation.
Primary Subtypes of POTS Include:
Neuropathic POTS
This form of POTS involves autonomic dysfunction, most notably affecting the neurocardiac axis, the critical communication pathway between the brain, heart, and blood vessels. In this condition, the nerves responsible for regulating vascular tone fail to function properly. As a result, when a person stands, blood vessels do not constrict effectively, causing blood to pool in the legs, arms, and abdomen.Hyperadrenergic POTS
This subtype is associated with excessive sympathetic nervous system activation, sometimes described as an exaggerated “fight or flight” response. Patients may experience adrenaline surges, shakiness, elevated heart rate, sweating, anxiety-like symptoms, palpitations, temperature sensitivity, and difficulty calming the system after stress or exertion.Hypovolemic POTS
Hypovolemic POTS is associated with reduced circulating blood volume. Patients may have difficulty maintaining adequate blood flow during upright posture, particularly during heat exposure, dehydration, illness, exercise, or prolonged standing. Common symptoms include fatigue, dizziness, exercise intolerance, weakness, heat intolerance, and feeling physically depleted after activity.Secondary POTS
Secondary POTS develops in association with another underlying condition or physiologic trigger. Some of the more common contributors evaluated include concussion and post-concussion syndrome, viral illness, Long COVID, connective tissue disorders or even significant physiologic stressors including surgery or trauma.Idiopathic POTS
Idiopathic POTS refers to cases where no single clearly identifiable underlying cause has been established. Patients may develop symptoms gradually or suddenly without a definitive triggering event such as concussion, viral illness, surgery, or autoimmune disease. The term “idiopathic” means that the exact cause remains uncertain, this does not mean symptoms lack a physiologic basis. Many patients still demonstrate measurable autonomic dysfunction involving circulation, cardiovascular regulation, exercise intolerance, blood pooling, sympathetic nervous system activation, or impaired physiologic recovery mechanisms.
POTS Clinical Insight
Many patients do not fit cleanly into a single subtype. Instead, they present with overlapping features that require a more individualized evaluation. In addition to these subtypes, some patients have overlapping conditions that can significantly influence symptoms and recovery, including:
Connective Tissue Disorders
Certain connective tissue disorders may contribute to autonomic dysfunction by impairing vascular support and blood vessel stability. One of the most commonly associated conditions is hypermobile Ehlers-Danlos Syndrome (hEDS), a disorder affecting connective tissue integrity throughout the body. This individuals may have blood vessels that are excessively elastic or less structurally supportive, making it more difficult to maintain normal vascular tone during upright posture. This can contribute to blood pooling, reduced blood return to the heart, and compensatory increases in heart rate.
Patients with connective tissue disorders may also experience joint hypermobility, chronic musculoskeletal pain, frequent sprains or injuries, cervical instability, and exercise intolerance. These overlapping features can significantly influence symptom presentation and recovery planning.
Mast Cell Activation and Overlapping Conditions
Some patients with POTS also demonstrate overlapping conditions involving mast cell activation, immune dysregulation, migraine disorders, gastrointestinal dysfunction, chronic fatigue presentations, vestibular dysfunction, or persistent post-viral symptoms. These overlapping physiologic contributors may complicate symptom patterns and influence activity tolerance, environmental sensitivity, recovery stability, and autonomic regulation.
Not every patient fits neatly into one category, and many individuals demonstrate overlapping physiologic patterns. Understanding these contributors is important because symptom drivers, recovery strategies, exercise tolerance, and rehabilitation planning may differ significantly between patients.
These factors can amplify symptoms and contribute to variability in presentation and response to care.
Learn more about the Types of POTS
Explore Concussion and Dysautonomia
Air Travel with POTS
Understand Mast Cell Activation and POTS
POTS Is Not a Single-System Condition
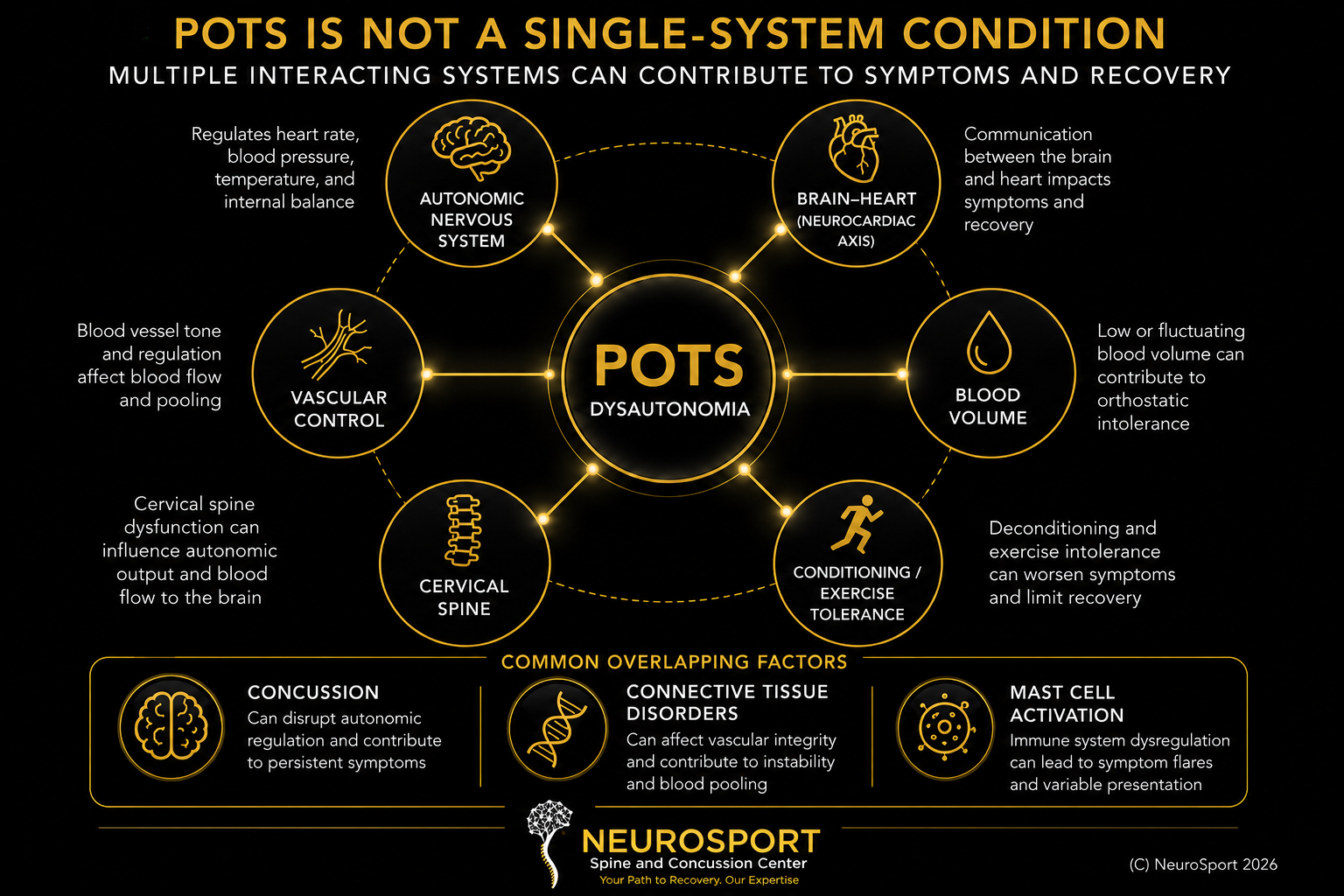
POTS and dysautonomia rarely involve a single isolated problem. In most patients, symptoms reflect overlapping autonomic dysfunction involving circulation, cognition, vision, blood pressure and pulse regulation, neurologic control, exercise/heat tolerance, recovery physiology, connective tissue integrity, immune regulation, or post-concussion and post-viral changes.
Dysautonomia frequently involves altered blood flow within the brain, particularly a condition known as cerebral hypoperfusion (a reduced or inadequate supply of blood to the brain.
This is one reason symptom patterns can and most commonly do vary significantly between individuals and why many patients continue struggling despite prior evaluation or treatment. The individual areas of the brain that are under supplied will drive which symptoms are presenting.
Less blood flow leads to decreased oxygenation and lowered rule access to that part of the brain.
The NeuroSport, assessment is designed to identify these interacting physiologic contributors in order to guide more targeted, individualized care.
The NeuroSport Approach to POTS and Dysautonomia Care
Care at NeuroSport is structured, system-based, and guided by clinical findings. Evaluation is designed to identify the specific factors contributing to symptoms, rather than applying generalized treatment approaches.
1. Identify the Drivers
Evaluation is designed to determine which systems are contributing to symptoms, including autonomic regulation, cardiovascular response, neurologic function, and cervical spine involvement.
This includes detailed history, symptom pattern recognition, and focused clinical examination.
2. Quantify Dysfunction
Objective testing is used to understand how the body is responding under physiologic demand.
This may include:
Orthostatic testing, including the NASA Lean Test
Heart rate and blood pressure response patterns
Symptom tracking and clinical scales
Functional tolerance to activity and positional change
Quantifying dysfunction allows for more precise clinical decision-making and tracking of progress over time.
3. Guide Targeted Recovery
Care is directed based on the patient’s specific presentation and tolerance.
This may include:
Structured autonomic rehabilitation using the Moreau POTS Protocol™
Graduated exercise progression based on physiologic response
Cervical spine mobilization when indicated
Symptom-guided activity modification and progression
What Makes This Different
Care at NeuroSport is designed for patients with persistent, complex symptoms who have not improved with standard approaches.
CORE DIFFERENTIATORS
We do not treat symptoms in isolation
Care is focused on identifying and addressing the underlying drivers of symptoms rather than simply managing them.
Evaluation is structured to identify the systems driving symptoms, not just the symptoms themselves
Assessment is structured to evaluate autonomic, neurologic, cardiovascular, and cervical contributors.
Care is guided by objective findings and physiologic response, not assumptions
Treatment is guided by clinical findings and physiologic response, not assumptions.
Integrated neurocardiac approach
Care focuses on the relationship between the brain, heart, and vascular system, rather than isolated symptoms.
Experience with complex cases
Many patients seen at NeuroSport have not improved with prior evaluation or treatment.
Patients are often seen after not improving with standard approaches and are seeking a more structured, system-based evaluation.
This approach allows for targeted, individualized care designed to improve function
and support recovery.
Conditions That Commonly Overlap with POTS
POTS often does not occur in isolation. Many patients have additional conditions that influence symptoms, recovery patterns, and response to care. Recognizing these overlapping factors is an important part of understanding the full clinical picture.
Common Overlapping Conditions Include:
Post-concussion autonomic dysfunction
Concussion can disrupt autonomic regulation and contribute to persistent symptoms such as dizziness, exercise intolerance, and heart rate instabilityConnective tissue disorders
Conditions such as hypermobility syndromes can affect vascular integrity and contribute to blood pooling and autonomic instabilityMast cell activation
Immune system dysregulation can lead to symptom flares, food sensitivities, heat intolerance, and variable symptom patterns
Why This Matters
These conditions can amplify symptoms, create variability in presentation, and make recovery less predictable when not identified. In many cases, patients are not dealing with a single diagnosis, but a combination of interacting systems that require a coordinated approach to evaluation and care.
At NeuroSport, these overlapping factors are considered as part of a structured, system-based evaluation to better define the drivers of symptoms and guide more effective care.
Learn more about Concussion and Dysautonomia
Learn more about Connective Tissue Disorders
Learn more about Mast Cell Activation and POTS
Who This Is For
Care at NeuroSport is designed for patients whose symptoms are persistent, complex, or not fully explained by standard evaluation.
This may be appropriate if:
You have been diagnosed with POTS but continue to have significant symptoms
You suspect dysautonomia but have not received clear answers
Your symptoms fluctuate and do not follow a predictable pattern
You experience dizziness, lightheadedness, or heart rate changes with standing
You have exercise intolerance or difficulty returning to activity
You have persistent symptoms following a concussion
You have not improved with prior treatment or evaluation
Patients Commonly Seen Include:
Individuals with POTS or suspected POTS
Patients with dysautonomia following concussion or illness
Athletes attempting to return to sport with unresolved symptoms
Individuals with complex or overlapping conditions affecting autonomic function
and are seeking a more structured, system-based approach to understanding and managing their condition.
Many patients seen at NeuroSport have already undergone prior evaluation and are often seen after not improving with standard approaches.
Many are seeking a more structured, system-based evaluation.
Request a Comprehensive Evaluation
If your symptoms have been persistent, difficult to explain, or have not improved with standard approaches, a structured evaluation may help identify the underlying drivers and guide a more targeted plan.
At NeuroSport, care begins with a comprehensive assessment designed to evaluate autonomic function, cardiovascular response, neurologic involvement, and contributing factors such as concussion history or overlapping conditions.
Most patients seen have already undergone prior evaluation and are seeking a more precise, system-based approach.
Next Steps
Schedule a comprehensive evaluation
Complete intake forms prior to your visit
Begin structured assessment and care planning

