
POTS and Heat
Why Symptoms Get Worse and How to Stay Functional
Heat is one of the most common and predictable triggers for POTS and dysautonomia symptoms.
If you feel worse in warm environments, there is a physiological reason; and a way to manage it.
Why Heat Hits Harder with POTS and Dysautonomia
Most people feel uncomfortable in the heat.
Patients with POTS and dysautonomia feel significantly worse, often within minutes. This is not a tolerance issue. It is a physiology issue.
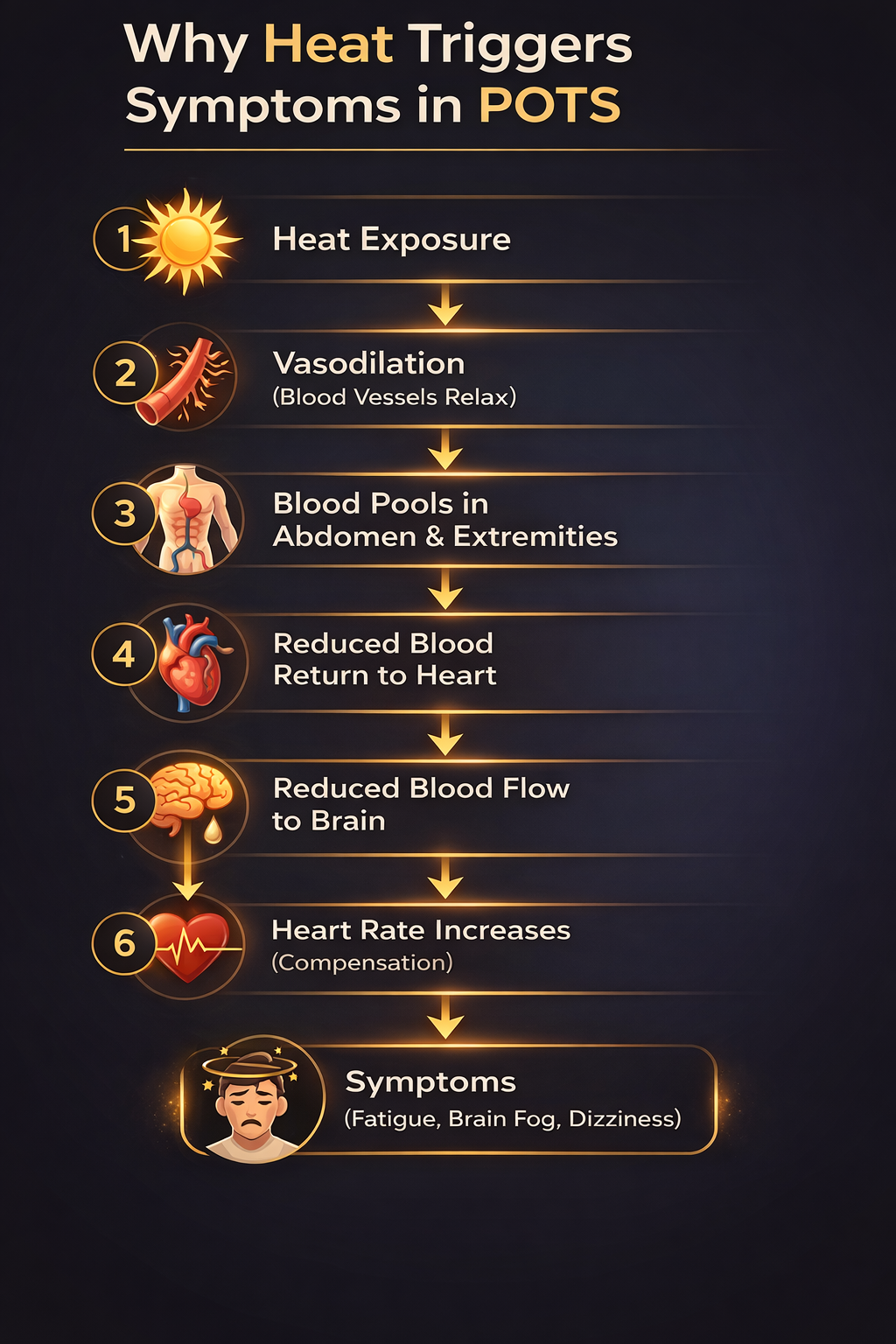
When your body is exposed to heat, blood vessels naturally dilate to help release your body’s heat. In a healthy system, the autonomic nervous system compensates by tightening other vessels and to maintain stable blood flow availability to the brain.
In POTS and dysautonomia, that system may not working efficiently.
The result:
Blood vessels remain too relaxed
Blood pools in the abdomen and extremities
Less blood returns to the heart
Less blood reaches the brain
To compensate, your heart rate increases rapidly in an attempt to maintain circulation. This is why patients commonly experience:
Lightheadedness
Fatigue
Brain fog
Increased heart rate
A general sense of “crashing” in warm environments
For many patients, heat is not just uncomfortable. It is one of the most consistent triggers of symptom flare-ups.
If symptoms reliably worsen in heat, that is a strong clinical clue that autonomic regulation is impaired.
Common Situations Where Heat Triggers Symptoms
Most patients do not notice heat intolerance in a controlled environment. They notice it when symptoms show up in real life. These situations are predictable. Once you see the pattern, it becomes easier to manage.
Common Triggers
Hot showers or baths
Hot tubs and saunas (can be dangerous)
Warm rooms with poor air circulation
Outdoor heat, especially mid-day or direct sun exposure
Standing in lines or crowded environments
Cooking over a stove or oven
Travel, especially airports and airplanes
Wearing heavy or non-breathable clothing
What These Situations Have in Common
Each of these environments increases:
Body temperature which leads to:
Blood vessel dilation and blood pooling:
Circulatory demand is not met because of the diversion of the blood to he skin
In a system already struggling to regulate blood flow, this creates a rapid shift in physiology. The result is often:
Sudden fatigue
Lightheadedness or dizziness
Increased heart rate
Brain fog or difficulty concentrating
Intolerance to hot environments
Key Insight
These episodes are not random! They are pattern-based physiological responses to heat and circulation stress. Once people recognize these patterns, they can begin to:
anticipate symptoms
modify exposure
and maintain better day-to-day function
What You Can Do to Stay Functional in the Heat
You do not have to avoid heat completely, but you do need to manage it strategically.
The goal is simple: Maintain circulating blood volume, reduce excessive heat load, and prevent rapid drops in blood flow to the brain.
1. Hydration: This Is Not Optional!
Start hydrating with electrolytes early. Do not wait until you feel symptoms.
Increase overall fluid intake throughout the day
Ensure you add electrolytes, not just water
Drink well before exposure to heat, and after exsposure
Hydration supports blood volume, which is critical for maintaining circulation.
2. Use Electrolytes to Support Circulation
For many POTS patients, increasing sodium, potassium and magnesium intake helps expand the blood volume to assist fluid retention and improve blood volume. The more blood you have the greater your ability to sweat and maintain blood flow.
Do more than just “Add salt to meals”
Use electrolyte solutions with glucose and adequate sodium
Avoid sugar free electrolytes; you uses glucose to increase sodium absorption
Be consistent, not occasional
This is one of the simplest and most effective strategies.
3. Control Your Environment When Possible
Small changes in environment can prevent large symptom swings.
Use fans or air conditioning
Avoid peak heat hours whenever possible
Sit instead of stand in warm environments
Take breaks before symptoms escalate
Dress to both shield your body from the sun
Control what you can. It makes a difference.
4. Modify Activity, Not Just Intensity
Heat increases cardiovascular demand.
Shorten duration of activity
Break activity into smaller segments
Avoid prolonged standing
Exercise in the cooler part of the day when possible
This is not about doing less. It is about doing it smarter.
5. Use Cooling Strategies
External cooling can reduce internal stress.
Cold water on the face or neck
Cooling towels or ice packs
Cold showers (brief, not prolonged hot exposure)
Lightweight, breathable clothing
Even small reductions in body temperature can improve symptoms.
6. Know When to Stop
Pushing through symptoms usually makes things worse.
If you feel:
dizzy
weak
mentally foggy
or your heart rate escalating
Stop, sit or lie down, hydrate, and cool your system.
Key Takeaway
Patients who do well in the heat are not avoiding it entirely. They are managing physiology in real time.
When Heat Intolerance Signals a Bigger Problem
Heat intolerance is common in POTS and dysautonomia. But in some cases, it is a sign that the system is not being adequately regulated. If symptoms are frequent, severe, or limiting daily function, it should not be dismissed as something you simply “live with.”
Signs That Warrant Further Evaluation
Symptoms occur with minimal heat exposure
You are unable to tolerate routine daily activities
Episodes are becoming more frequent or more intense
Heart rate increases rapidly with minimal stress
Symptoms do not improve with hydration and basic strategies
You feel near-syncope or actually faint
What This May Indicate
These patterns often reflect:
Reduced blood volume
Impaired vascular tone
Poor autonomic regulation
Inadequate physiological adaptation to stress
In other words, the system is struggling to maintain stability even under normal conditions.
Clinical Perspective
Heat intolerance is not the condition. It is a signal.
When that signal is strong or persistent, it points to underlying autonomic dysfunction that may benefit from targeted evaluation and structured management.
What to Do Next
If heat consistently disrupts your ability to function:
Seek evaluation from a provider experienced in POTS and dysautonomia
Undergo objective assessment of heart rate, blood pressure, and autonomic response
Develop a structured plan that goes beyond basic lifestyle adjustments
Key Takeaway
You should not have to organize your life around avoiding heat.
With the right approach, most patients can improve tolerance, stabilize symptoms, and regain function.
Bottom Line: Managing Heat with POTS
Heat is one of the most reliable triggers of symptoms in POTS and dysautonomia.
The reason is not unclear.
It is rooted in how the body regulates blood flow, temperature, and circulation.
What Matters Most
Heat increases vascular dilation and circulatory demand
The autonomic system struggles to compensate
Symptoms follow predictable physiological patterns
What Works
Stay ahead of hydration and sodium intake
Control your environment when possible
Modify activity based on conditions
Use simple cooling strategies
Recognize early symptoms and respond quickly
What to Remember
These symptoms are not random.
They are not in your head.
And they are not something you simply have to tolerate.
They are manageable with the right approach.
Final Thought:
Patients who understand their physiology make better decisions, respond earlier to symptoms, and maintain a higher level of function.
That is the goal.
Persistent Symptoms? Get Answers.
If you are experiencing dizziness when standing, rapid heart rate, fatigue, or symptoms that have not improved with prior care, a structured autonomic evaluation may help identify the underlying cause.

