
Why Do I Feel Dizzy When I Stand Up?
Many patients with POTS are told their symptoms are due to anxiety.
While anxiety can cause physical symptoms, POTS is a disorder of the autonomic nervous system that affects heart rate, blood flow, and physiological regulation.
Understanding the difference is critical, as the underlying mechanisms and treatment approaches are not the same.
In POTS, symptoms are often triggered by physiological stressors such as standing, heat, or prolonged activity, rather than emotional factors. Recognizing these patterns allows for a more accurate clinical evaluation and helps guide patients toward appropriate care pathways.
You’re Not Alone, and This Is Not “Just Anxiety”
Many patients with these symptoms are initially told their condition is anxiety-related. While anxiety can contribute to symptoms, it is often not the primary cause.
At NeuroSport, many patients arrive after seeing multiple providers without clear answers. Our focus is identifying the underlying cause of symptoms through structured clinical evaluation.
What Happens in Your Body When You Stand Up?
When you stand, your body must rapidly adjust to gravity
by maintaining blood flow to the brain.
In patients with autonomic dysfunction:
Blood vessels may not adjust their size effectively
Blood pools in the exstremities and abdomen
Less blood is available to returns to the heart
Heart rate then must increases to compensate
for decreased circulating blood
This can result in:
Dizziness or lightheadedness
Rapid heart rate or palpitations
Fatigue
Brain fog
Fainting or near fainting
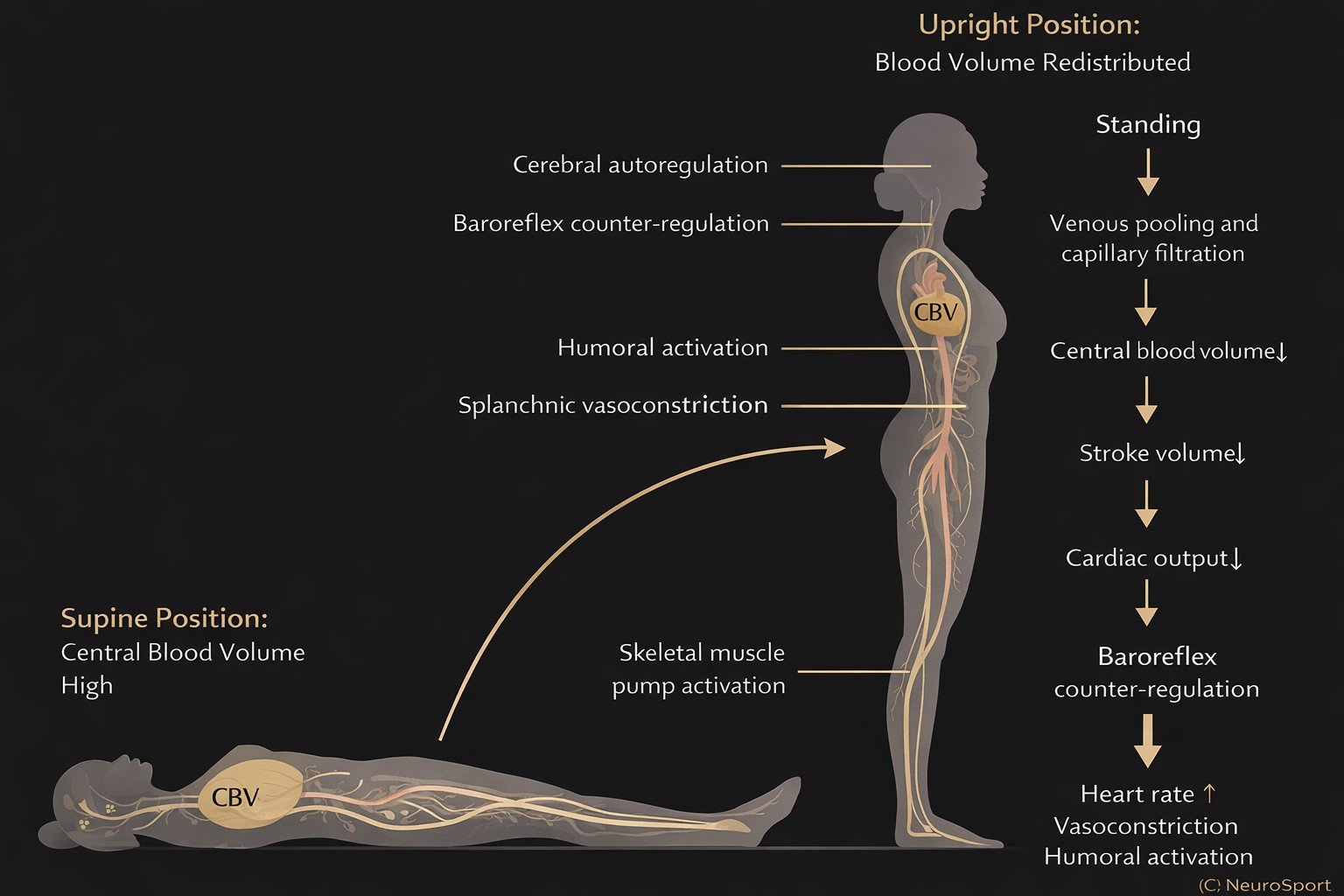
How Blood Flow Changes When You Stand
This diagram illustrates how reduced central blood volume and
compensatory heart rate changes contribute to symptoms.
Clinical Insight
Dizziness when standing is often not a primary heart problem. In many cases, the heart is responding appropriately to reduced blood return caused by impaired vascular regulation.
Common Causes of ANS Related Dizziness When Standing
Postural Orthostatic Tachycardia Syndrome (POTS)
A condition where heart rate increases excessively when standing, often with fatigue and cognitive symptoms.
Orthostatic Hypotension
A significant drop in blood pressure upon standing. May associated with dysautonomia.
Post-Concussion Autonomic Dysfunction
Decreased blood flow through the injured part of the brain secondary to autonomic regulation following head injury.
Deconditioning and Volume Dysregulation
Reduced blood volume or conditioning contributing to symptoms.
Symptoms may worsen with heat, prolonged standing, or exertion.
How NeuroSport Evaluates These Symptoms
Evaluation is focused on identifying the underlying cause through structured clinical assessment.
Detailed clinical history
Orthostatic testing (NASA Lean Test when indicated)
Heart rate and blood pressure response analysis
Assessment of autonomic function
Evaluation for contributing factors including concussion
Specialized Evaluation at NeuroSport
Care is led by William J. Moreau, DC, DACBSP, FACSM, with extensive experience in autonomic dysfunction and complex neurologic presentations. Evaluation focuses on identifying physiologic drivers of symptoms and guiding targeted rehabilitation.
Experiencing sudden worsening of symptoms?
You may be dealing with a dysautonomia flare.
→ Learn what causes flares and how to recover → Dysautonomia Flares page
How These Conditions Are Treated
Treatment is based on individual findings and tailored to each patient.
Autonomic rehabilitation strategies
Structured exercise progression (Moreau POTS Protocol)
Hydration and electrolyte strategies
Cervical spine management when indicated
Gradual return to activity
Dizziness When Standing Is Often Treatable
These symptoms are commonly misunderstood, but with the right clinical approach, meaningful improvement is possible.
At NeuroSport, care is focused on identifying the underlying cause and guiding patients through a structured path to recovery.
Learn more about our approach to POTS and dysautonomia care here.
Persistent Symptoms? Get Answers.
If you are experiencing dizziness when standing, rapid heart rate, fatigue, or symptoms that have not improved with prior care, a structured autonomic evaluation may help identify the underlying cause.
The Moreau POTS Protocol (MPP™)
The Moreau POTS Protocol is a structured, clinically guided program designed to restore autonomic regulation through targeted exercise and physiologic progression.

