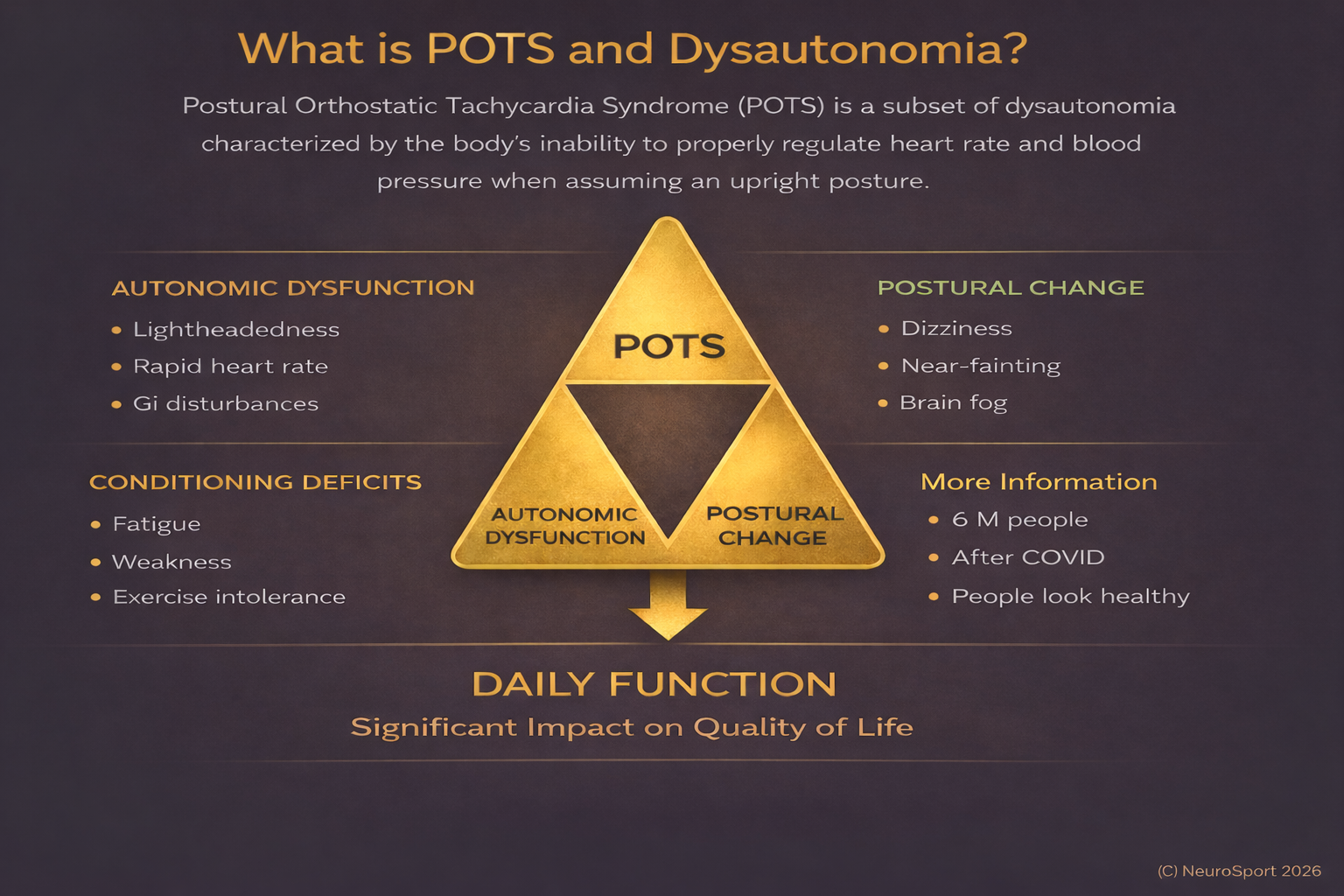
What are Different Types of POTS?
This visual reflects how autonomic dysfunction and postural changes combine to impact daily function.
What is POTS?
POTS is not simply a heart rate issue. It is a disorder of autonomic regulation involving the coordination between the brain, heart, and blood vessels. This reflects dysfunction of the autonomic driven neurocardiac axis, the communication system that regulates circulation and cardiovascular response to posture.
When this system is not functioning properly, blood does not circulate effectively when upright. Blood can pool in the lower body, reducing blood flow to the brain and triggering a compensatory increase in heart rate.
Patients with POTS often experience a wide range of symptoms, including lightheadedness, fatigue, palpitations, cognitive dysfunction, and exercise intolerance. Symptoms are frequently worse with standing, heat, dehydration, or after meals.
Although POTS is sometimes misunderstood or misattributed to anxiety, it is a measurable and diagnosable condition involving dysfunction of the autonomic nervous system.
Patients with POTS commonly experience:
• Lightheadedness
• Fatigue
• Palpitations
• Brain fog
• Exercise intolerance
Symptoms are often worse with:
• Standing
• Heat
• Dehydration
• After meals
Not all patients fit neatly into a single category. Many present with overlapping features across multiple POTS patterns.
👉 See how we evaluate these patterns clinically: → POTS Evaluation and Care
Although POTS is often misunderstood or misattributed to anxiety, it is a measurable condition involving dysfunction of the autonomic nervous system.
👉 Learn more about how this system works: → Understanding the Brain-Heart Connection
The Autonomic Nervous System: POTS at Its Core
The autonomic nervous system (ANS) regulates essential body functions such as heart rate, blood pressure, circulation, digestion, and temperature control. These processes occur automatically and are critical for maintaining stability during daily activities, especially when changing posture.
The ANS has three divisions:
Sympathetic nervous system – prepares the body for activity by increasing heart rate and constricting blood vessels
Parasympathetic nervous system – supports recovery and balance by slowing heart rate and promoting restorative processes
Enteric nervous system - a complex "second brain" that regulates digestion, motility, immune responses, and fluid secretion
In POTS, this system becomes dysregulated. Blood vessels may not constrict effectively when standing, leading to blood pooling in the lower body. As a result, less blood returns to the heart and brain, and the body compensates by increasing heart rate. This mismatch between vascular control and cardiac response is a key driver of symptoms.
Common clinical effects include reduced exercise tolerance, rapid fatigue, cognitive impairment, and heightened physiologic stress response.
POTS is not a single uniform condition. While all patients meet similar diagnostic criteria, the underlying drivers can differ significantly. Identifying these patterns is critical, as they influence both symptom presentation and treatment strategy.
The Primary Forms of POTS
The following subtypes represent the most commonly observed patterns in clinical practice. Many patients demonstrate overlap between categories, and accurate evaluation focuses on identifying the dominant contributing factors. Overlapping Features: POTS rarely exists as a single subtype. Most patients demonstrate a combination of patterns, requiring a broader clinical lens.
Clinical Prevalence: Neuropathic and hyperadrenergic features are commonly identified, often coexisting within the same patient. One of the most common forms of POTS seen at NeuroSport is “Secondary POTS”. Secondary POTS occurs as a result of an underlying conditions, often multiple conditions, like autoimmune diseases (e.g., Lupus, Sjögren's), diabetes, or connective tissue disorders (e.g. Ehlers-Danlos Syndrome (EDS) or hypermobility disorders.
Neuropathic POTS
Impaired nerve function affects the body’s ability to constrict blood vessels, leading to blood pooling in the lower extremities and reduced circulation to the brain. This subtype is associated with dysfunction of the peripheral autonomic nerves and may be seen in patients with prior illness, injury, or neurologic involvement, including head injury. Learn More
Hyperadrenergic POTS
Increased sympathetic nervous system activity results in elevated circulating stress hormones, contributing to excessive heart rate, blood pressure variability, and heightened physiologic arousal. Patients may also report symptoms such as anxiety, tremulousness, and reduced tolerance to stress.
Hypovolemic POTS
Reduced blood volume limits effective circulation, contributing to fatigue, dizziness, and reduced exercise tolerance. In these patients, inadequate circulating volume places additional strain on cardiovascular regulation when upright.
Secondary POTS
POTS develops in association with another underlying condition. Common contributors include underlying medical conditions, connective tissue disorders, post-viral syndromes, and head injury (concussion). In these cases, addressing the underlying condition is often an important component of care.
Autoimmune-Related POTS
In some patients, POTS is associated with immune system dysregulation. This may involve the presence of autoantibodies that affect autonomic nerve signaling or vascular control. Autoimmune-related POTS is often seen following illness or infection and may present with fluctuating or persistent symptoms not fully explained by cardiovascular changes alone.
Idiopathic POTS
Idiopathic POTS is diagnosed when a patient clearly meets criteria for POTS, but there is no identifiable underlying condition is driving it.
Why identifying your POTS subtype matters
Identifying the underlying drivers of POTS is essential for effective care. While symptoms may appear similar across patients, the mechanisms can differ significantly. Without this distinction, treatment is often inconsistent or ineffective.
Improves diagnostic accuracy and clinical clarity
Guides targeted treatment strategies
Reduces trial-and-error management
Helps patients better understand their condition
At NeuroSport, evaluation is focused on identifying these patterns through objective testing and clinical correlation, allowing care to be directed at the root of the problem rather than just symptom control.
Evaluation of POTS requires more than identifying changes in heart rate. A comprehensive, systems-based approach is necessary to identify the underlying contributors to autonomic dysfunction and persistent symptoms.
Treatment Approach
At NeuroSport Spine and Concussion Center, evaluation is structured, in-depth, individualized, and includes:
Comprehensive clinical history with symptom pattern analysis and contributing factor identification
Detailed physical and neurologic examination, including assessment of cervical, vestibular, and autonomic function
Testing for POTS including the NASA Lean Test with continuous heart rate and blood pressure monitoring
Assessment of physiologic responses to positional change and autonomic stress
Targeted laboratory and functional testing when clinically indicated
Integration of findings across autonomic, neurologic, and cardiovascular systems to guide diagnosis and care planning
Following evaluation, care is guided by clinical findings and may include structured progression using the Moreau POTS Protocol (MPP), along with individualized strategies targeting identified contributors to autonomic dysfunction.
You’re Not Alone—And Answers Are Available
Over 6 million Americans have POTS. The number of people with POTS significantly increased after the COVID crisis. POTS is not an easy diagnosis. Patients with POTS often experience persistent and unexplained symptoms that can significantly impact daily life. A structured evaluation can help identify contributing factors and guide a more targeted approach to care.
If you are experiencing symptoms such as dizziness, fatigue, palpitations, or exercise intolerance, further evaluation may be appropriate.
👉 If you are experiencing symptoms such as dizziness, rapid heart rate, fatigue, brain fog, or exercise intolerance, it is important to understand that these are not random. They are often the result of measurable dysfunction within the autonomic nervous system.
What to Do If This Sounds Familiar
If you’ve been trying to understand your symptoms and the pieces have not fully come together, that is common.
Many patients we see have been evaluated for individual symptoms without a clear explanation of how those symptoms are connected.
POTS and dysautonomia require a systems-based evaluation that looks at how the autonomic nervous system is functioning in real time.
A structured evaluation can help identify whether POTS or another form of dysautonomia is present, and more importantly, determine the underlying drivers contributing to your symptoms.
Comprehensive clinical history and symptom analysis
Objective autonomic and physiologic testing
Identification of contributing patterns and subtype features
Development of a targeted, individualized care plan
When properly evaluated, these conditions are not only diagnosable, they are manageable with the right approach.
Related Reading
If you are exploring POTS and dysautonomia, these resources provide additional insight into common patterns, triggers, and management strategies:
Not All POTS Is the Same: Understanding the 5 Types of POTS
Why You Feel Worse After Eating: Dysautonomia and Blood Flow
Nutrition Strategies for Dysautonomia and POTS
The Brain–Heart Connection in Autonomic Dysfunction
Understanding the condition is the first step. Identifying your pattern is where progress begins.
Related Reading
Author
William J. Moreau, DC, DACBSP, FACSM