Post-Concussion Syndrome
Why Symptoms Persist and What to Do Next
Persistent Post-Concussion Symptoms (PPCS) lacks a universally accepted definition, and the term itself is increasingly being replaced by “persistent post-concussion symptoms (PPCS)” to reflect a more accurate understanding of prolonged recovery. Rather than representing a single condition, these persisting symptoms in head injured individuals often reflect multiple interacting systems that have not fully recovered following injury.
If you are still dealing with symptoms weeks or months after a concussion you’re not alone and you’re not imagining it. Many patients continue to experience headaches, dizziness, brain fog, fatigue, and difficulty tolerating daily activities long after the initial injury.
These symptoms are real and often reflect ongoing dysfunction in the brain, autonomic nervous system, and cervical spine—not simply a delayed recovery.
NeuroSport evaluates patients with persistent post-concussion symptoms from across North America.
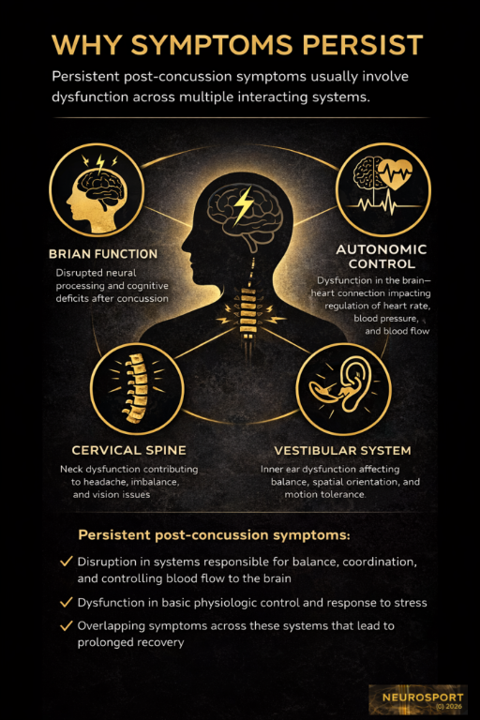
Why Concussion Symptoms Persist
Persistent post-concussion symptoms lasting more than 4 weeks after injury, when typical recovery is expected within 2-3 weeks is the first indicator the patient is not going to experience the expected recovery trajectory.
Persistent symptoms after a concussion are not random. In many cases, these persisting symptoms reflect ongoing neurological driven dysfunction across multiple systems initially affected at the time of injury rather than a single unresolved issue. These persistent symptoms can and commonly do adversely impact the patient’s quality of life.
Recovery from concussion may not always linear. While many individuals improve within a few weeks, a meaningful percentage continue to experience symptoms beyond the expected recovery window. These persistent symptoms are now more accurately described in the medical literature as persistent post-concussion symptoms (PPCS), reflecting a shift away from the idea of a single “syndrome” and toward a more complex, multi-system model of recovery.
When the underlying contributors are not identified and addressed, symptoms may persist despite time, rest, and standard care.
Key Contributors to Persistent Symptoms
Persistent symptoms often involve a combination of the following:
Autonomic nervous system dysfunction
Impaired regulation of heart rate, blood pressure, and blood flow can contribute to dizziness, fatigue, brain fog, and exercise intolerance.
👉 Learn more about this pattern in POTS and dysautonomia →Cervical spine dysfunction
Injury to the neck can contribute to headaches, dizziness, visual symptoms, and altered proprioception, often overlapping with other systems.Vestibular dysfunction
Disruption of balance and spatial orientation systems can lead to dizziness, motion sensitivity, and instability.Oculomotor dysfunction
Impaired eye tracking and coordination can affect reading, screen tolerance, focus, and concentration.Neurometabolic and physiologic changes
Altered brain energy use and blood flow regulation following injury require targeted identification of affected systems rather than passive observation.
Why This Matters
Persistent symptoms may indicate ongoing lack of resolution of the head injury. They often reflect dysfunction within systems that were affected at the time of injury. These systems interact closely, and when one is impaired, it can disrupt others, creating a cycle of ongoing symptoms.
Identifying which systems are involved is the key to effective treatment.
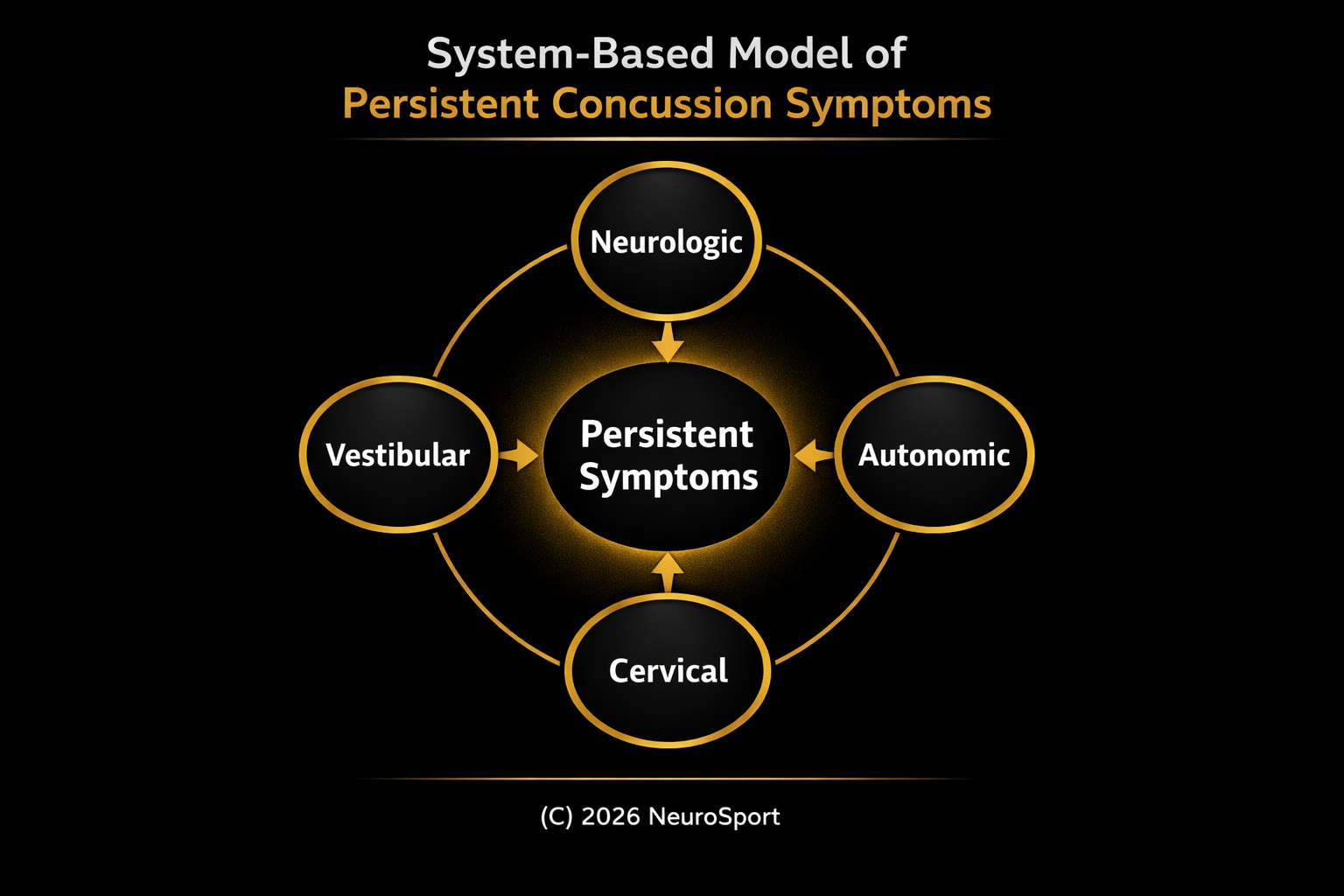
Common Symptoms of Post-Concussion Syndrome
Symptoms persisting beyond 2–4 weeks may reflect persistent post-concussion symptoms (PPCS), a multi-system condition requiring targeted evaluation.
At NeuroSport, evaluation is structured and system-based, focusing on the underlying contributors to persistent symptoms rather than symptoms alone.
Neurologic function
Autonomic nervous system regulation
Cervical spine function
Vestibular and balance systems
Oculomotor (eye movement) control
Exercise tolerance and physiologic response
No single test defines post-concussion syndrome. Effective evaluation requires integration across multiple clinical domains to identify the primary drivers of symptoms.
Symptoms following a concussion can vary widely and often involve multiple systems. Rather than occurring in isolation, they typically present as a pattern that reflects dysfunction across physical, cognitive, and emotional domains.
The type, severity, and combination of symptoms differ between individuals and may change over time, particularly in response to activity, stress, or environmental factors.
Symptoms persisting beyond 2–4 weeks may reflect persistent post-concussion symptoms (PPCS), a multi-system condition requiring targeted evaluation. At NeuroSport, evaluation is structured and system-based, focusing on the underlying contributors to persistent symptoms rather than symptoms alone.
Neurologic function
Autonomic nervous system regulation
Cervical spine function
Vestibular and balance systems
Oculomotor (eye movement) control
Exercise tolerance and physiologic response
No single test defines post-concussion syndrome. Effective evaluation requires integration across multiple clinical domains to identify the primary drivers of symptoms.
Symptom Domains
Persistent post-concussion symptoms are commonly grouped into the following categories:
Physical / Somatic
Headache
Dizziness or imbalance
Sensitivity to light or noise
Fatigue
Neck pain
Cognitive
Brain fog or slowed thinking
Difficulty concentrating
Memory difficulties
Reduced processing speed
Emotional / Behavioral
Irritability
Mood changes
Increased stress sensitivity
Sleep / Recovery
Difficulty falling or staying asleep
Non-restorative sleep
Daytime fatigue
Symptom Behavior
Symptoms are often not constant. Instead, they tend to follow recognizable patterns:
Worsening with physical exertion
Increased symptoms with cognitive demand
Fluctuation throughout the day
Sensitivity to environmental stimuli such as light, noise, or busy settings
These patterns can provide important clues about which systems are contributing to ongoing symptoms.
Clinical Perspective
Persistent symptoms are not random. Their pattern often reflects underlying dysfunction in systems such as the autonomic nervous system, cervical spine, vestibular system, and oculomotor control.
Understanding how symptoms cluster and respond to stressors is a key part of identifying the drivers of prolonged recovery.
What We Evaluate
At NeuroSport, evaluation is structured, system-based, and focused on identifying the underlying contributors to persistent symptoms rather than simply documenting symptoms alone.
Because post-concussion symptoms often involve multiple interacting systems, effective assessment requires integration across neurologic, physiologic, and functional domains.
Clinical Evaluation Framework
The evaluation process focuses on the following key areas:
👉 Neurologic function
Assessment of cognitive performance, processing speed, and overall neurologic integration to identify deficits in brain function following injury.
👉 Autonomic nervous system regulation
Evaluation of heart rate, blood pressure, and blood flow control, particularly in response to postural change and activity.
Dysfunction in this system can contribute to dizziness, fatigue, brain fog, and exercise intolerance.
👉 See how this relates to POTS and dysautonomia →
👉 Cervical spine function
Assessment of joint motion, neuromuscular control, and symptom reproduction related to the cervical spine.
This is a common but often overlooked contributor to headache, dizziness, and visual symptoms.
👉 Vestibular and balance systems
Evaluation of postural stability, spatial orientation, and motion sensitivity to identify balance-related contributors to symptoms.
👉 Oculomotor (eye movement) control
Assessment of eye tracking, convergence, and visual coordination.
Deficits in this system commonly affect reading, screen tolerance, and cognitive endurance.
👉 Exercise tolerance and physiologic response
Evaluation of how the body responds to graded physical activity, including heart rate response, symptom provocation, and recovery patterns.
Integrated Clinical Approach
No single test defines post-concussion syndrome or persistent post-concussion symptoms.
Effective evaluation requires integration of findings across multiple domains to identify:
The primary drivers of symptoms
Secondary contributing factors
Interactions between systems
This approach allows for a more precise understanding of the condition and provides the foundation for targeted, individualized care.
Clinical Perspective
Persistent symptoms are not explained by a single deficit.
They reflect disruption in systems that regulate:
Brain function
Blood flow
Movement
Balance
Physiologic response to stress
Identifying how these systems interact is essential to guiding recovery.
Our Approach to Care:
Targeted Evaluations Leading to Individualized Treatment
Treatment for persistent post-concussion symptoms is most effective when it is directed at the specific systems contributing to ongoing dysfunction.
Because symptoms often arise from multiple interacting systems, care is individualized and progresses based on physiologic response rather than a fixed timeline.
Treatment Is Based on Identified Drivers
Autonomic rehabilitation may incorporate structured, monitored protocols designed to progressively restore physiologic control and improve tolerance to activity. At NeuroSport, treatment is guided by findings from a structured evaluation and may include the following:
👉 Cervical spine rehabilitation
When dysfunction is identified, targeted cervical spine mobilization and neuromuscular rehabilitation are used to address contributors to headache, dizziness, and visual symptoms.
👉 Autonomic rehabilitation
Interventions are designed to improve regulation of heart rate, blood pressure, and blood flow.
This may include graded cardiovascular activity and structured protocols to restore autonomic control and improve exercise tolerance.
👉 Vestibular rehabilitation
Targeted exercises are used to improve balance, reduce motion sensitivity, and restore spatial orientation.
👉 Oculomotor rehabilitation
Exercises focused on eye tracking, convergence, and visual coordination help improve reading tolerance, screen use, and cognitive endurance.
👉 Graded activity progression
Return to physical and cognitive activity is guided by physiologic response rather than symptom avoidance alone, allowing for controlled and progressive recovery.
Integrated, System-Based Care
Persistent symptoms are rarely driven by a single factor. Treatment is coordinated across systems to address both primary and secondary contributors to dysfunction.
This integrated approach allows for:
More efficient recovery
Reduced symptom fluctuation
Improved tolerance to daily activity and exercise
Clinical Perspective
Recovery from persistent post-concussion symptoms requires more than time and rest.
It requires identifying the systems involved and applying targeted interventions that restore function across those systems.
When treatment is directed at the underlying drivers, meaningful progress becomes possible. This approach aligns with current evidence supporting a multi-system, targeted model for persistent post-concussion symptoms.
The Role of Autonomic Dysfunction
In many patients, persistent symptoms following concussion are driven in part by dysfunction of the brain–heart connection, commonly referred to as the neurocardiac axis.
This system plays a critical role in regulating heart rate, blood pressure, and blood flow, particularly during changes in posture and physical activity. When this system is disrupted, the body may have difficulty maintaining stable circulation to the brain, resulting in a range of symptoms that can persist well beyond the initial injury.
Common Autonomic-Related Symptoms
Autonomic dysfunction may contribute to:
Exercise intolerance
Dizziness or lightheadedness, particularly with standing
Fatigue and reduced energy levels
Difficulty with prolonged upright posture
Brain fog or reduced mental clarity
Abnormal or exaggerated heart rate responses
These symptoms often follow recognizable patterns and may worsen with:
Physical exertion
Prolonged standing
Heat exposure
Cognitive demand
Post-Concussion Autonomic Dysfunction
Following concussion, disruption of autonomic regulation can impair the body’s ability to appropriately respond to physiologic stress.
This may result in:
Reduced efficiency of blood flow to the brain
Increased cardiovascular strain during activity
Fluctuating symptoms throughout the day
In some patients, this pattern may evolve into or reveal conditions such as postural orthostatic tachycardia syndrome (POTS) despite normal imaging.
👉Learn more about POTS and dysautonomia →
Clinical Perspective
Autonomic dysfunction is often under-recognized in patients with persistent post-concussion symptoms.
When present, it can significantly impact recovery by limiting tolerance to physical and cognitive activity.
Identifying and addressing dysfunction within the neurocardiac axis is a critical component of a comprehensive evaluation and targeted treatment approach.
Clinical Insight
Persistent post-concussion symptoms are not simply a prolonged recovery. In many cases, they reflect identifiable and treatable dysfunction across multiple interacting systems. When these contributors are accurately identified and addressed, meaningful improvement is often possible.
Current evidence supports dysfunction of the autonomic nervous system as an important contributor to persistent post-concussion symptoms. Newer research indicated that decreased blood flow to the injured part of the brain is a key factor in persistent concussion related brain dysfunction. This could in turn connect to the onset of the dysautonomia.
Following concussion, disruption of autonomic regulation can impair the body’s ability to control:
Heart rate
Blood pressure
Breathing patterns
Blood flow to the brain
Exercise tolerance
This dysregulation may contribute to symptoms such as:
Dizziness and orthostatic intolerance
Fatigue and reduced energy
Cognitive fog and decreased mental clarity
Exercise intolerance and symptom exacerbation with activity
Persistent symptoms after concussion are typically multifactorial.
However, autonomic dysregulation is now increasingly recognized as a key mechanism that should be considered during both clinical evaluation and targeted rehabilitation.
Clinical Perspective
Persistent symptoms are often maintained by physiologic dysfunction rather than structural injury alone.
Identifying and addressing these dysfunctions allows for a more targeted approach to care and improved recovery outcomes.
When to Seek a Specialized Evaluation
At NeuroSport, evaluation is focused on patients who are not recovering as expected following concussion.
If symptoms persist or recovery has plateaued, a structured, system-based evaluation is often necessary to identify the underlying contributors and guide targeted care. Findings are based on objective physiologic response rather than symptom report alone.
NeuroSport evaluates patients from across the United States with persistent and complex post-concussion symptoms.
You May Benefit from a Specialized Evaluation If:
Symptoms persist beyond 2–4 weeks following injury
You have not improved with prior care or treatment approaches
Symptoms worsen with physical or cognitive activity
You experience ongoing dizziness, fatigue, or exercise intolerance
You are having difficulty returning to work, school, or sport
Symptoms fluctuate or do not follow a clear recovery pattern
Why This Matters
Persistent symptoms are often treatable when the underlying causes are properly identified.
Without a structured evaluation, contributing factors such as autonomic dysfunction, cervical involvement, or vestibular deficits may go unrecognized.
What to Expect
A comprehensive evaluation at NeuroSport is designed to:
Identify the primary drivers of your symptoms
Clarify contributing physiologic and functional factors
Establish a clear, individualized plan for recovery
The goal is not simply to manage symptoms, but to understand what is causing them and address those factors directly.
Next Step
If you are not progressing as expected after a concussion, further evaluation may provide important clarity and direction.
Use the “Request an Evaluation” link below to get started on your return to health.

