Why Is My MRI Normal After a Concussion?
Concussion and Persistent concussion symptoms exist even when CT scans and MRI studies appear “normal.”
A concussion is primarily a "functional" injury. While a CT scan can show if the brain's "building" is intact, it cannot see if the "electricity" or cellular communication inside is failing.
One of the Most Common Questions We Hear
Many concussion patients are told:
“Your MRI is normal.”
“Your CT scan looks fine.”
“There is nothing structurally wrong.”
Yet these patients may still experience very real symptoms such as:
Brain fog
Dizziness
Head pressure
Exercise intolerance
Light sensitivity
Fatigue
Rapid heart rate
Visual motion sensitivity
Difficulty concentrating
Poor stress tolerance
Sleep disturbance
Autonomic dysfunction
This creates understandable confusion and frustration. Patients often begin wondering:
“If my scan is normal, why do I still feel terrible?”
“Am I imagining this?”
“Did the doctors miss something?”
At NeuroSport, we spend a great deal of time helping patients understand an important concept:
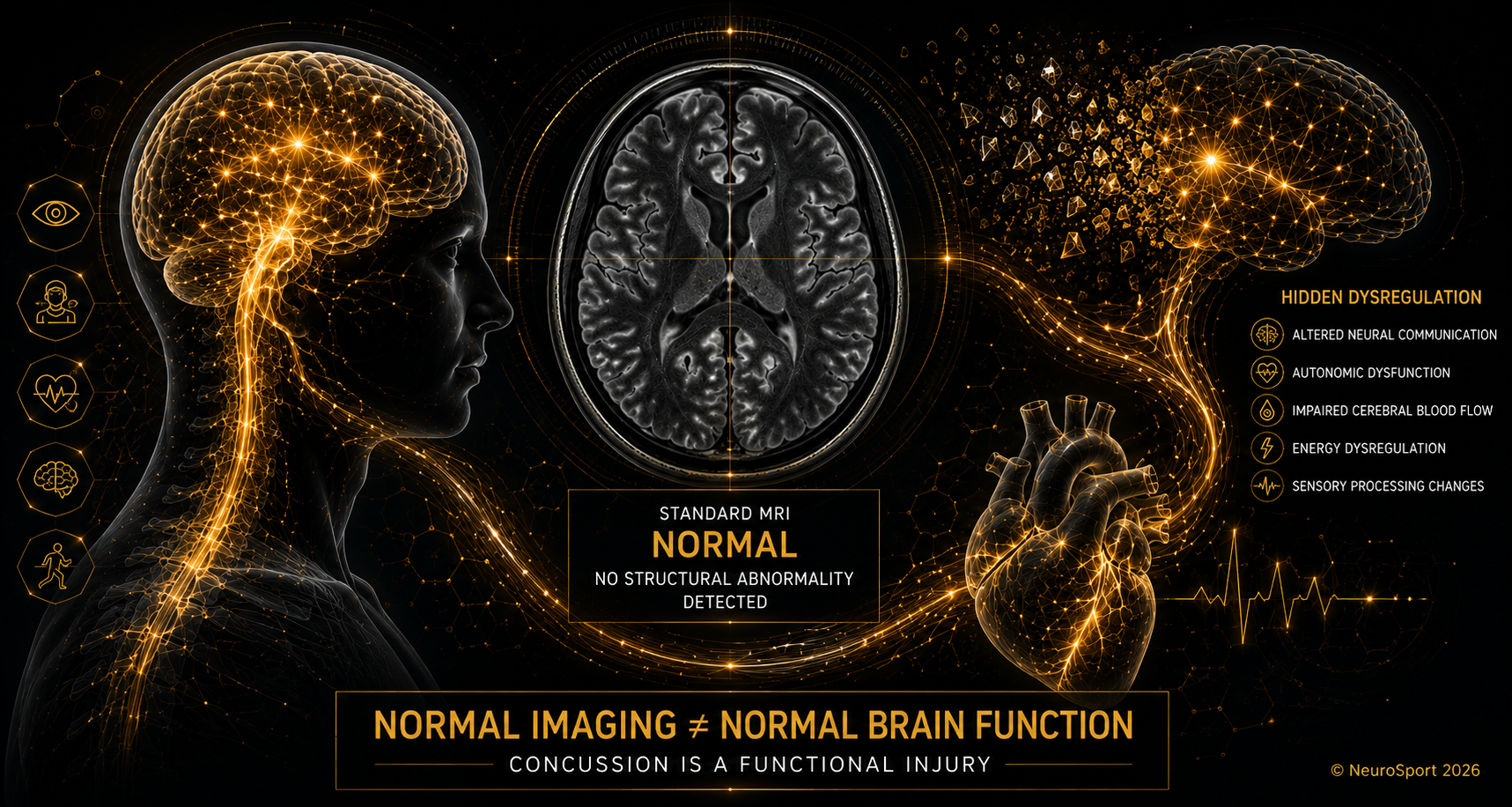
A concussion is primarily a functional injury, not a large structural injury visible on standard imaging.
What CT and MRI Scans Are Designed to Detect
Standard CT and MRI imaging are extremely important medical imaging tools. These studies are designed primarily to identify structure injuries like:
Bleeding
Skull fractures
Stroke
Tumors
Brain swelling
Structural damage
Large tissue abnormalities
These scans are critically important in evaluating the brain for emergency medicine and trauma care. However, concussion involves “neurometabolic” changes; microscopic and physiologic dysfunctions. These changes occur below the resolution of standard imaging technologies.
In many concussion cases:
brain cells remain physically present
no large bleed exists
no major structural lesion is visible
Yet the brain’s ability to regulate and communicate efficiently may still be impaired.
Concussion Often Involves Functional Brain Dysfunction
Concussion may disrupt:
Neural communication
Energy metabolism
Cerebral blood flow regulation
Autonomic nervous system regulation
Neurovascular coupling
Sensory processing
Exercise tolerance systems
Oculomotor control
Vestibular integration
This is why patients may experience significant symptoms despite “normal” imaging.
At NeuroSport, we commonly explain this concept using a simple analogy:
A computer may look completely normal from the outside while the software operating system is malfunctioning internally.
The hardware appears intact.
The function is impaired.
Why Symptoms Can Persist
Persistent symptoms are unique to the individuals injury and their individual characteristics. The portion or more commonly portions of the brain that is injured drives the clinical presentation. After concussion may reflect ongoing dysfunction involving:
Cerebral blood flow regulation
Autonomic nervous system balance
Exercise intolerance
Vestibular dysfunction
Oculomotor dysfunction
Cervical spine injury
Sleep dysregulation
Neuroinflammatory responses
Sensory integration dysfunction
For some patients, concussion may also trigger:
Dysautonomia
Neurogenic POTS
Brain cognitive dysfunction
Orthostatic intolerance
Migraine disorders
Persistent post-traumatic headache
This is one reason two patients both with an injury named “concussion” typically have different symptoms and may recover very differently.
Advanced Imaging Research
Some imaging tools are primarily used in research may be able to image concussion in the future. These imaging tools are typically outside the generally accessible imaging methods available to diagnosticians. Imaging tools that have demonstrated promise in imaging abnormalities include:
Functional MRI (fMRI)
PET scanning
SPECT imaging
Diffusion tensor imaging (DTI)
These technologies may identify:
altered blood flow
metabolic changes
connectivity disruption
white matter changes
However, many of these technologies are still used primarily in research settings and are not routinely relied upon for standard concussion diagnosis.
At NeuroSport, concussion diagnosis remains primarily based on:
clinical history
symptom patterns
neurologic examination
autonomic assessment
physiologic testing
functional evaluation
Objective Evaluation Matters
At NeuroSport, we focus on identifying measurable signs of dysfunction that may contribute to persistent symptoms. Depending on the patient presentation, evaluation may include:
Detailed history
Cranial nerve examination
Orthostatic vital signs
NASA Lean Test
Exercise tolerance assessment
Oculomotor examination
Vestibular assessment
Cervical spine evaluation
Symptom burden analysis
Activity intolerance profiling
Heart rate response analysis
The goal is not simply to say:
“Your imaging is normal.”
The goal is to understand:
WHY symptoms persist and what systems may still be dysregulated.
In many concussion and post-concussion cases, standard CT or MRI imaging is normal. That does not mean the injury is not real. It means the injury may not be visible on routine structural imaging. At NeuroSport, we help identify and document the functional evidence of brain injury and post-concussion dysfunction through a detailed clinical evaluation.
This can be important for two reasons:
Patients often need confirmation that their symptoms are real, measurable, and clinically meaningful.
Legal cases often require clear documentation connecting the injury event to persistent functional impairment.
Our evaluation may include objective and semi-objective findings such as:
Concussion mechanism and acute symptom onset
Symptom evolution over time
Neurologic examination findings
Oculomotor dysfunction
Vestibular impairment
Balance deficits
Cognitive screening abnormalities
Autonomic dysfunction
Orthostatic intolerance
Exercise intolerance
Cervical injury findings
Headache pattern analysis
Functional limitations
Response to graded exertional testing
Recovery trajectory over time
The goal is not to “force” a diagnosis. The goal is to determine whether the history, symptom pattern, examination findings, physiologic testing, and functional limitations are medically consistent with concussion or post-concussion syndrome.
For medical-legal cases, this type of evaluation can help address important questions, including:
Was there a plausible mechanism for concussion?
Did symptoms begin or worsen after the injury event?
Are the patient’s symptoms consistent with known concussion presentations?
Are there objective clinical findings supporting ongoing dysfunction?
Are there overlapping injuries, such as cervical, vestibular, or autonomic dysfunction?
Is the recovery course medically reasonable?
Are future care needs supported by clinical findings?
Recovery Is Still Possible
Normal imaging does not mean symptoms are imagined. It also does not mean recovery is impossible. Many concussion patients improve substantially when contributing physiologic systems are appropriately identified and addressed.
Recovery may involve:
Structured autonomic rehabilitation
Exercise progression
Vestibular rehabilitation
Oculomotor rehabilitation
Cervical spine management
Sleep optimization
Hydration and sodium strategies
Activity pacing
Dysautonomia management
At NeuroSport, rehabilitation plans are individualized based on the patient’s neurologic and autonomic presentation.
Persistent Symptoms After Concussion Deserve Careful Evaluation
If you continue struggling with dizziness, fatigue, brain fog, exercise intolerance, rapid heart rate, or autonomic symptoms despite “normal” imaging, further evaluation may help identify contributing physiologic dysfunction.
NeuroSport provides focused assessment and rehabilitation for complex concussion and post-concussion autonomic presentations.

