Mast Cell Activation and POTS
When immune system dysregulation amplifies autonomic symptoms
Many patients with POTS and dysautonomia experience symptoms that seem unpredictable, inconsistent, or difficult to explain. Symptoms may flare suddenly, worsen after meals, increase in heat, or vary dramatically from day to day.
Mast Cell Activation Syndrome (MCAS) and Postural Orthostatic Tachycardia Syndrome (POTS) frequently overlap, with MCAS acting as an underlying, treatable driver for POTS symptoms in some patients. In MCAS, faulty immune cells inappropriately release mediators like histamine, causing inflammation, flushing, and gastrointestinal distress that can trigger or worsen the dizziness, tachycardia, and fatigue typical of POTS.
MCAS has been implicated since chemical mediators released from mast cells may cause symptoms suggestive of POTS (postural tachycardia, lightheadedness).
In some individuals, mast cell activation may contribute to this instability and amplify autonomic dysfunction.
Why POTS Symptoms Can Feel So Unpredictable
Many patients with POTS and dysautonomia describe symptoms that seem inconsistent, difficult to predict, or disproportionate to everyday activities.
Symptoms may:
flare suddenly
change dramatically from one day to the next
appear unrelated to exertion or activity level
For some individuals, these fluctuations may involve overlapping inflammatory and autonomic system dysfunction. Patients often describe:
episodes of rapid heart rate or lightheadedness
flushing or temperature sensitivity
food or medication sensitivities
gastrointestinal discomfort or nausea
fatigue and cognitive fog that vary throughout the day
periods of relative stability followed by sudden physiologic “crashes” or flares
These patterns can be frustrating because symptoms may not follow a predictable course and may not always appear during standard medical testing.
In some patients, mast cell activation may contribute to this physiologic instability and amplify autonomic symptoms. Mast cell-related dysfunction has been associated with inflammatory signaling, vascular instability, orthostatic intolerance, gastrointestinal symptoms, and neuroinflammatory processes.
At NeuroSport, these symptom patterns are evaluated within the broader context of interacting autonomic, neurologic, vascular, and inflammatory systems.
What Is Mast Cell Activation?
Mast cells are part of the immune system and play an important role in inflammatory and allergic responses. When activated appropriately, mast cells help the body respond to threats such as infection or injury. However, in some individuals, mast cells may become overly reactive or dysregulated, releasing excessive inflammatory mediators such as:
Histamine
Prostaglandins
Leukotrienes
Cytokines
These substances can influence multiple body systems simultaneously, including:
Blood vessel regulation
Heart rate response
Gastrointestinal function
Temperature regulation
Neurologic and inflammatory signaling
Because these effects involve multiple systems, mast cell activation may contribute to symptoms that appear inconsistent, widespread, or difficult to explain. Mast cell activation has been associated with overlapping conditions including:
POTS and dysautonomia
Hypermobility syndromes
Chronic migraines
Irritable bowel symptoms
Post-viral syndromes
Persistent neuroinflammatory presentations
Importantly, mast cell-related symptoms are often episodic and may fluctuate significantly over time. Symptoms may become more noticeable during physiologic stress, illness, heat exposure, poor sleep, emotional stress, or autonomic flares.
At NeuroSport, mast cell activation is considered as one possible overlapping contributor within a broader systems-based evaluation of autonomic dysfunction and symptom instability.
Why Mast Cell Activation Matters in POTS
POTS is not simply a heart rate disorder. In many patients, symptoms involve interacting autonomic, vascular, neurologic, and inflammatory systems.
Mast cell activation may amplify autonomic dysfunction by contributing to:
Blood vessel dilation and vascular instability
Increased blood pooling
Fluctuating heart rate responses
Heat intolerance
Gastrointestinal dysregulation
Neuroinflammatory signaling
Increased symptom variability and physiologic sensitivity
These overlapping mechanisms may help explain why some patients experience:
sudden symptom flares
inconsistent day-to-day tolerance
worsening symptoms after meals
increased sensitivity to heat or environmental triggers
disproportionate fatigue following relatively minor activity
Mast cell mediators such as histamine and tryptase may also influence neuroinflammatory pathways and autonomic regulation. Mast cells have been shown to interact with neurologic and immunologic signaling systems that may contribute to symptom amplification in complex dysautonomia presentations.
Importantly, not every patient with POTS has mast cell activation, and not every patient with mast cell activation has POTS. However, these conditions commonly overlap and may contribute to more complex or fluctuating symptom patterns.
At NeuroSport, evaluation focuses on identifying these overlapping contributors and understanding how multiple systems may be interacting within the broader clinical presentation.
What Are Mast Cells?
Mast cells are immune system cells that help protect the body. They are found throughout the body, especially in the skin, blood vessels, airways, gastrointestinal tract, and tissues near nerves.
When mast cells detect a threat, they can release chemical messengers called mediators. These include histamine, prostaglandins, leukotrienes, cytokines, and other inflammatory signaling molecules.
These mediators affect several body systems at the same time, including:
Skin and flushing responses
Blood vessel tone and blood pressure regulation
Heart rate and autonomic responses
Gastrointestinal function
Temperature regulation
Neurologic symptoms such as headache, sensory sensitivity, and brain fog
This is why mast cell activation can look confusing. It may not present as a simple “allergy.” Instead, it may appear as a multi-system flare involving skin, circulation, digestion, and autonomic symptoms.
Common Symptom Patterns
Patients with overlapping mast cell activation and dysautonomia often describe symptoms that fluctuate across multiple body systems rather than following a single predictable pattern.
Common symptom patterns:
Autonomic and Cardiovascular
Rapid heart rate or palpitations
Lightheadedness when standing
Heat intolerance
Blood pooling sensations
Episodic worsening of orthostatic symptoms
Exercise intolerance or poor recovery
Neurologic and Cognitive
Brain fog
Fatigue that fluctuates significantly
Head pressure or headaches
Sensory overstimulation
Increased symptom sensitivity during stress or illness
Gastrointestinal
Nausea
Abdominal discomfort or bloating
Symptoms worsening after meals
Food-related symptom triggers
Variable gastrointestinal tolerance
Inflammatory and Systemic
Flushing or temperature dysregulation
Increased sensitivity to medications or environmental exposures
Symptom flares during physiologic stress
Symptoms that appear disproportionate or inconsistent
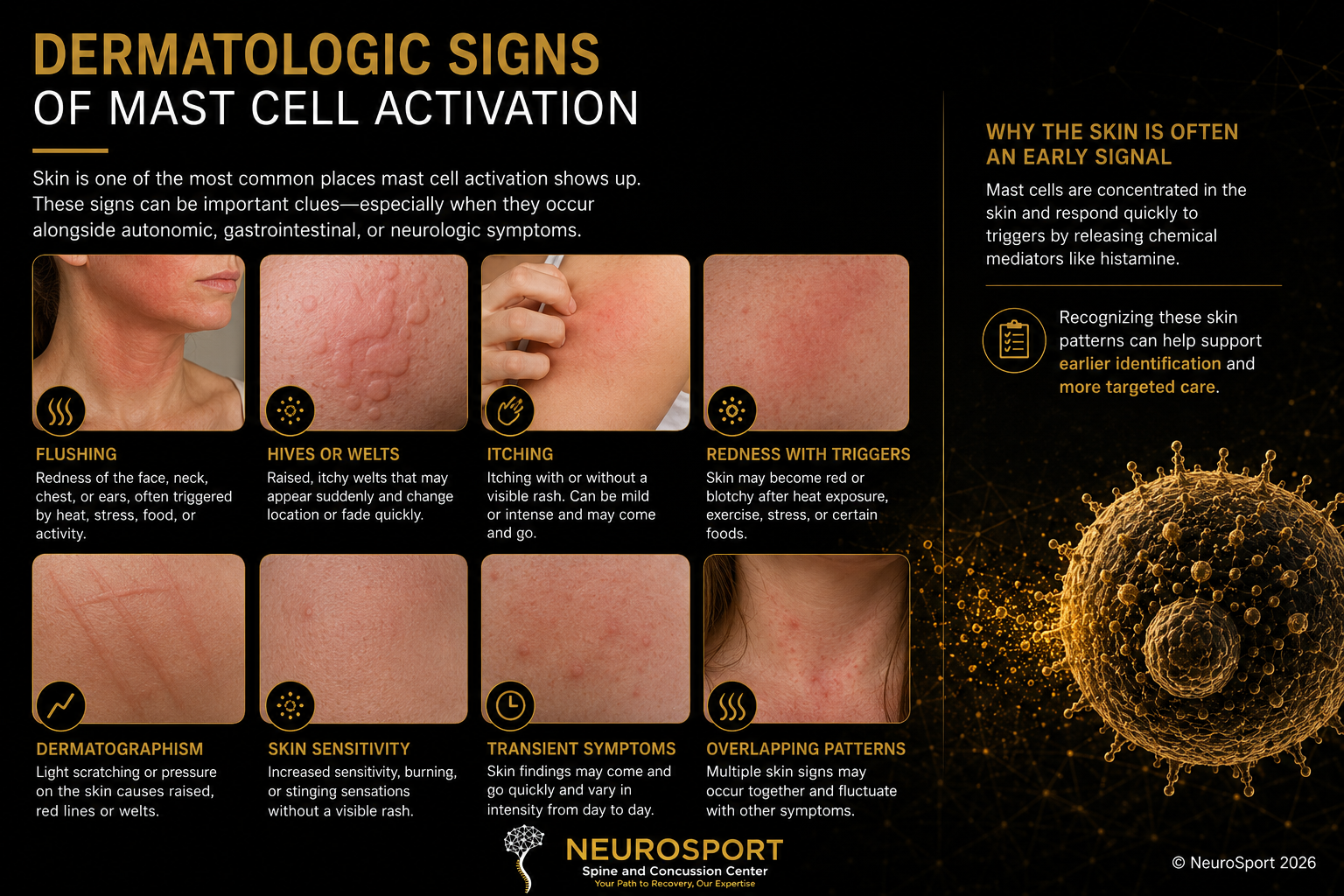
Skin and Dermatologic Findings
Mast cell activation may involve visible or sensory skin symptoms, including:
Flushing of the face, neck, chest, or ears
Itching with or without a visible rash
Hives or transient welts
Redness after heat, stress, food exposure, or exercise
Skin sensitivity or burning sensations
Dermatographism, where light scratching or pressure produces raised red marks
These skin findings can be important clinical clues, especially when they occur alongside dizziness, rapid heart rate, GI symptoms, heat intolerance, or unexplained flares. Many patients report periods of relative stability followed by sudden symptom escalation without an obvious explanation.
These fluctuating patterns can make diagnosis challenging and may contribute to delayed recognition of overlapping autonomic and inflammatory dysfunction.
Why These Types of Cases Are Often Missed
Many patients with overlapping mast cell activation and dysautonomia undergo extensive evaluation while continuing to struggle with persistent or fluctuating symptoms.
One reason these cases are often difficult to recognize is that symptoms may:
involve multiple body systems simultaneously
fluctuate significantly over time
worsen during intermittent flares
appear inconsistent during standard office visits or testing
In some patients, laboratory findings may also be variable or normal outside of active symptom episodes.
Because symptom patterns are complex and often episodic, patients are sometimes told:
testing is normal
symptoms are stress-related or anxiety-related
symptoms are inconsistent or difficult to explain
symptoms do not fit a single diagnosis
In reality, many patients may be experiencing overlapping physiologic dysfunction involving autonomic regulation, vascular control, inflammatory signaling, and neurologic system interaction.
At NeuroSport, these presentations are approached through a broader systems-based framework designed to identify contributing patterns rather than focusing on isolated symptoms alone.
Why Response to Antihistamines May Matter
For some patients, improvement with mast cell-directed treatment may provide an important clinical clue. This may include response to:
H1 antihistamines
H2 blockers
Leukotriene-modifying medications
Mast cell stabilizing strategies, when appropriate
A positive response does not automatically confirm mast cell activation, and treatment decisions should be individualized. However, when symptoms are consistent with mast cell activation and improve with targeted therapy, that response may help support the clinical picture.
This is especially relevant because mast cell-related laboratory findings can fluctuate, may depend on timing during a flare, and may be affected by specimen handling. Clinical history, symptom patterns, laboratory data, and treatment response all need to be interpreted together.
Bottom line
The page is good, but it currently assumes too much patient knowledge. Add:
What mast cells are
What mast cells do
How activation gets dysregulated
Derm findings
Antihistamine response as a clinical clue
NeuroSport Clinical Approach
At NeuroSport, evaluation is designed to identify patterns of dysfunction and understand how autonomic, neurologic, vascular, and inflammatory systems may be interacting within the broader clinical presentation.
Instead of focusing on a single isolated diagnosis, assessment considers the possibility of overlapping contributors that may amplify symptom burden and physiologic instability.
Evaluation may include:
Detailed symptom and flare history
Orthostatic and autonomic assessment
Review of food, heat, environmental, and activity-related triggers
Assessment of exercise and recovery tolerance
Evaluation of overlapping contributors such as concussion history or connective tissue disorders
Review of symptom variability and physiologic response patterns
When clinically appropriate, laboratory studies may also be ordered to help evaluate for mast cell-related dysfunction or other overlapping contributors to autonomic instability.
Depending on the clinical presentation, this may include evaluation of inflammatory mediators or other laboratory markers associated with mast cell activation. Because mast cell-related findings may fluctuate over time, laboratory interpretation is considered within the broader clinical context and symptom pattern.
Because mast cell-related symptoms may fluctuate significantly over time, identifying patterns and triggers is often an important part of the clinical process.
At NeuroSport, the goal is not simply symptom management, but improved physiologic stability, better functional tolerance, and more consistent day-to-day performance across interacting body systems.
Related Topics
Mast cell activation may overlap with several other conditions and symptom patterns commonly evaluated at NeuroSport.
POTS and Dysautonomia Care
Concussion and Dysautonomia
Connective Tissue Disorders and Dysautonomia
These related topics can help patients better understand how autonomic, inflammatory, neurologic, and vascular systems may interact in complex presentations.
Request an Evaluation
If symptoms are persistent, unpredictable, or difficult to explain, a structured autonomic evaluation may help identify contributing factors and guide a more targeted care plan.
At NeuroSport, assessment is designed to evaluate autonomic regulation, physiologic response patterns, overlapping contributors, and the interaction between neurologic, vascular, inflammatory, and cardiovascular systems.
Many patients seen at NeuroSport have already undergone prior evaluation and are seeking a more structured, systems-based approach to understanding persistent symptoms. If you think you may have mast cell activation problems or POTS and would like answers take the next step!
Next Steps
Request a comprehensive evaluation
Complete intake forms prior to your visit
Begin structured assessment and individualized care planning

