
Concussion Can Disrupt the
Autonomic Nervous System
Persistent symptoms after concussion may reflect dysfunction of the brain-heart connection, not simply “slow recovery.”
Concussion Can be More Than a Brain Injury
Many people think concussion affects only memory, headaches, or concentration. In reality, concussion that does not resolve in a week or two can also disrupt the autonomic nervous system, the system responsible for regulating heart rate, blood pressure, circulation, temperature control, digestion, and exercise tolerance.
At NeuroSport, we commonly evaluate patients whose persistent post-concussion symptoms are strongly linked to autonomic dysfunction.
These patients may experience:
Dizziness when standing
Rapid heart rate
Exercise intolerance
Brain fog
Heat intolerance
Fatigue
Lightheadedness
Palpitations
Nausea
Temperature dysregulation
Poor recovery after activity
Cognitive overload after minimal exertion
For some patients, concussion acts as the triggering event that disrupts autonomic regulation and leads to conditions such as:
Post-concussion autonomic dysfunction
Neurogenic POTS
Orthostatic intolerance
Dysautonomia
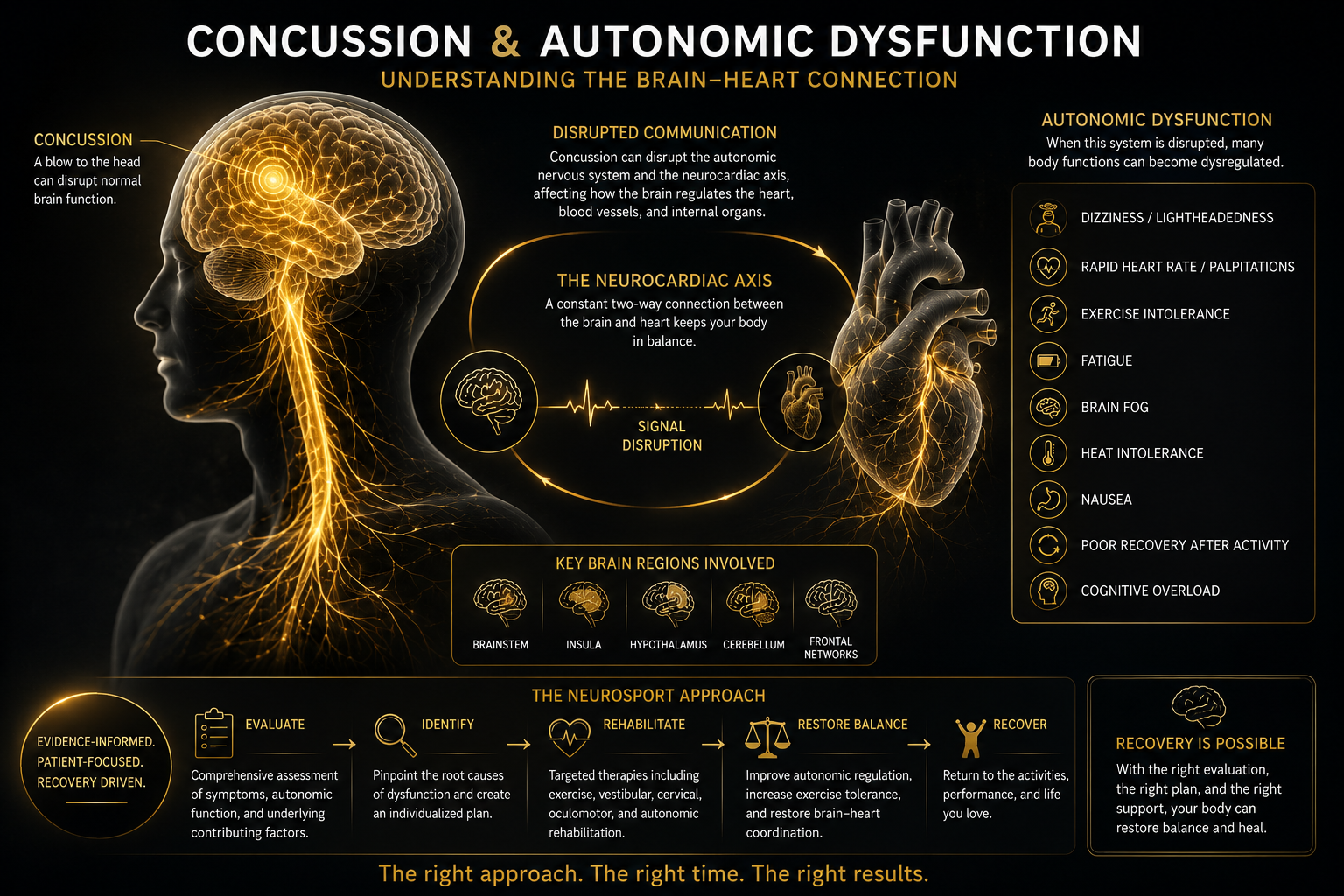
The Brain-Heart Connection
The autonomic nervous system relies on constant communication between the brain and cardiovascular system. This communication network is sometimes referred to as central control or the neurocardiac axis. After concussion, this system may become dysregulated.
Areas of the brain involved in autonomic control include:
Brainstem
Insular cortex
Hypothalamus
Cerebellum
Frontal regulatory networks
When these systems are disrupted, the body may struggle to appropriately regulate circulation and physiologic demand. This can result in:
Excessive heart rate increases when standing
Blood pooling in the extremities
Reduced cerebral blood flow
Exercise intolerance
Symptom flares after cognitive or physical exertion
Increased sensitivity to stressors such as heat, dehydration, or sensory overload
At NeuroSport, we frequently explain this to patients as a disruption of the body’s “automatic regulation system.”
Why Symptoms Persist
One of the most frustrating experiences for patients is being told that imaging is “normal” despite ongoing symptoms. Concussion-related autonomic dysfunction often does not appear on standard CT or MRI imaging.
Yet patients may continue struggling with:
Daily fatigue
Orthostatic intolerance
Cognitive overload
Dizziness
Exercise intolerance
Visual motion sensitivity
Head pressure
Tachycardia
Poor stress tolerance
This does not mean symptoms are psychological or imagined. Instead, it often reflects physiologic dysregulation involving:
Cerebral blood flow regulation
Heart rate control
Vascular tone
Autonomic balance
Exercise recovery systems
Neuroinflammatory responses
At NeuroSport, we focus heavily on identifying objective signs of dysfunction to help guide rehabilitation and recovery planning.
What Has Changed in Concussion Management?
Concussion care has evolved significantly over the past decade. Many older recommendations are no longer considered best practice. At NeuroSport, we emphasize evidence-guided concussion management that reflects modern understanding of brain injury, autonomic dysfunction, and recovery physiology.
Earlier Evaluation Matters!
Research increasingly supports early assessment by clinicians experienced in concussion management, especially in younger patients. Earlier identification of contributing factors such as:
Autonomic dysfunction
Vestibular dysfunction
Oculomotor dysfunction
Cervical spine injury
Exercise intolerance
Examining the injured patient for these dysfunctions may help reduce prolonged recovery trajectories and improve rehabilitation planning.
Prolonged Sensory Deprivation Is No Longer Recommended
Years ago, patients were often advised to remain in dark rooms with strict avoidance of screens, light, sound, reading, and activity for extended periods.
Modern concussion care has moved away from prolonged sensory deprivation.
While temporary reduction of symptom-provoking stimulation may be appropriate early after injury, excessive isolation and inactivity may actually contribute to:
Deconditioning
Increased anxiety
Sleep disruption
Autonomic dysregulation
Delayed recovery
Appropriate Exercise Has Become an Important mainstay to Recovery
Carefully supervised aerobic exercise is now widely recognized as an important rehabilitation tool for many concussion patients. The goal is not maximal exertion. The goal is controlled physiologic rehabilitation that supports recovery of autonomic and neurologic regulation.
Patients Should Not Be Routinely Awakened Throughout the Night
A long-standing myth in concussion care involved repeatedly waking patients overnight after injury. Current recommendations do not support routinely awakening a stable concussion patient throughout the night if they have already undergone appropriate medical evaluation and no red-flag signs are present. If they need to be awakened in the night, they should be looked after in a hospital setting.
Sleep is critically important for neurologic recovery.
However, patients with worsening symptoms, neurological decline, repeated vomiting, severe deterioration, or concerning signs require immediate medical evaluation.
NeuroSport Comprehensive Concussion and Autonomic Evaluation
Our evaluations may include:
Detailed autonomic history
Orthostatic vital signs
NASA 10-Minute Lean Test
Heart rate response analysis
Exercise tolerance assessment
Oculomotor examination
Vestibular assessment
Cervical spine evaluation
Symptom burden analysis
Activity intolerance profiling
We also evaluate for overlapping contributors that may complicate recovery, including:
Neurogenic POTS
Connective tissue disorders
Hypermobility syndromes
Sleep dysfunction
Migraine disorders
Cervicogenic dysfunction
Persistent post-traumatic headache
Deconditioning
Dysregulated breathing patterns
Exercise Is One of the Most Powerful Tools in Concussion Recovery
For years, concussion patients were commonly told to rest in dark rooms, avoid activity, and wait for symptoms to resolve. There is no medication proved to treat concussion. While short-term rest may be appropriate immediately after injury, modern concussion management has evolved substantially. Today, research increasingly supports the idea that appropriately guided and supervised exercise can play a major role in recovery.
At NeuroSport, exercise is not viewed as “pushing through symptoms.” We use exercise strategically to help restore physiologic regulation and improve autonomic function. Based upon Dr. Moreau’s work at the United States Olympic Committee and innovations he brings with him from his work on the NFL’s International Thin Tank on Concussion Research our approach is safe, supervised and evidence guided. We know how to help.
After concussion, many patients develop impaired exercise tolerance due to dysfunction involving:
Cerebral blood flow regulation
Heart rate control
Autonomic nervous system balance
Neurovascular coupling
Exercise recovery physiology
This helps explain why some patients feel worse with physical or cognitive exertion, even months after injury. When exercise is carefully structured and progressed appropriately, it may help:
Improve autonomic regulation
Restore exercise tolerance
Improve cerebral blood flow dynamics
Reduce physiologic deconditioning
Improve energy regulation
Reduce symptom flares over time
Improve confidence with movement and activity
At NeuroSport, exercise progression is individualized based on symptom response, orthostatic tolerance, cardiovascular response, and overall neurologic presentation. For some patients, exercise becomes one of the most important turning points in recovery.
Rehabilitation Recovery Focus
Recovery from post-concussion autonomic dysfunction often requires a graded exercise protocol that beats rest alone recovery by weeks.
NeuroSport Concussion Management is evidence guided and includes:
Structured autonomic rehabilitation
Graduated exercise progression
Heart rate-guided training
The Moreau POTS Protocol™
Cervical spine rehabilitation
Oculomotor rehabilitation
Hydration and sodium strategies
Sleep optimization
Activity pacing
Autonomic flare management strategies
At NeuroSport, rehabilitation plans are individualized based on the patient’s symptom profile, physiologic tolerance, and autonomic presentation.
Persistent Symptoms After Concussion May Reflect More Than
“Slow Recovery”
Persistent symptoms after concussion are not always “just part of recovery.”
For many patients, unresolved autonomic dysfunction, exercise intolerance, cervical dysfunction, vestibular impairment, or neurophysiologic dysregulation continue to drive symptoms long after the initial injury.
NeuroSport provides focused evaluation and evidence-guided rehabilitation for complex concussion and post-concussion autonomic presentations.

